- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Stress In Teens? Ayurvedic Practices To Follow For Mental Clarity

Image Credit: Canva
In the modern world, overstimulation is a constant companion, affecting people across all age groups. Adolescents, navigating the complex transition from childhood to adulthood, are particularly vulnerable. This transformative phase is marked by curiosity, rapid growth, and numerous physical, emotional, and social developments. The challenges of adolescence often include managing stress, coping with hormonal changes, and building essential life skills such as problem-solving and self-confidence. Ayurveda, an ancient science of holistic wellness, offers solutions to help adolescents achieve balance and mental clarity during this crucial stage of life.
Adolescence is a time of both opportunity and challenge, where rapid changes can feel overwhelming for teenagers and their families. The physical transformations, emotional swings, and social pressures of this phase demand careful attention to health and well-being. Neglecting these needs can lead to long-term issues, including anxiety, depression, and unhealthy habits. Ayurveda provides a framework to address these concerns by integrating dietary recommendations, lifestyle adjustments, and mental health practices tailored to the unique needs of adolescents.
Emotional turbulence is one of the most common challenges during adolescence. Anxiety, excessive worry, nervousness, and irritability can hinder mental clarity and emotional growth. Depression, marked by persistent sadness, further complicates the journey to adulthood. These emotional challenges are often exacerbated by body image issues, disordered eating habits, and addiction. Many teenagers, especially girls, struggle with their self-image, experimenting with extreme diets or succumbing to eating disorders like anorexia nervosa. Others may turn to substance abuse or display antisocial behaviors, further distancing themselves from a healthy lifestyle.
To combat these challenges, Ayurveda emphasizes balance. Stress management is a cornerstone of Ayurvedic practice, offering tools like yoga, meditation, and breathing exercises. These practices help adolescents find inner calm, reduce stress levels, and foster mental clarity. By incorporating these techniques into daily routines, teenagers can build resilience and enhance their overall well-being.
Hormonal imbalances often accompany adolescence, contributing to mood swings and physical discomfort. Ayurveda recognizes the importance of balancing the doshas—Vata, Pitta, and Kapha—to restore harmony. Personalized diet plans, herbal remedies, and lifestyle adjustments can naturally regulate hormones, promoting emotional stability and vitality. Ancient Ayurvedic formulations like Medhya Rasayana—a group of herbs known for enhancing memory and intellect—are particularly beneficial during this phase. Ingredients like Mandukaparni (Centella asiatica), Guduchi (Tinospora cordifolia), and Brahmi (Bacopa monnieri) improve focus, alleviate stress, and nurture the restless mind.
Ayurvedic therapies such as Pizhichil and Shirodhara further enhance mental clarity and emotional stability during adolescence.
● Pizhichil, also known as the "king of Ayurvedic therapies," involves a gentle, rhythmic pouring of warm medicated oil over the entire body, combined with a synchronized massage. This procedure calms the nervous system, alleviates stress, and nourishes the body. For adolescents, Pizhichil can help soothe physical discomfort from growth spurts and hormonal imbalances while promoting deep relaxation.
● Shirodhara, another widely renowned therapy, involves the continuous pouring of warm herbal oil or buttermilk onto the forehead. This technique specifically targets mental agitation, relieving symptoms of anxiety, insomnia, and excessive worry. Shirodhara’s calming effects on the mind make it an ideal remedy for sensory overstimulation and emotional turbulence in teenagers.
The Ayurvedic approach also extends to everyday practices that support mental health. A nourishing diet is central to this philosophy. Warm, freshly prepared meals infused with herbs and spices like turmeric, cumin, and ginger enhance digestion and promote balance. Adolescents are encouraged to avoid processed and raw foods, stay hydrated, and maintain regular meal times. Proper sleep, another vital aspect, plays a critical role in cognitive function and emotional regulation. Inadequate rest can impair focus, exacerbate anxiety, and weaken immunity.
Ayurveda also underscores the importance of caring for the senses. Adolescents often experience sensory overstimulation, which can disrupt their mental equilibrium. Simple practices like taking breaks during school or work, resting the eyes, and spending time in nature help soothe the senses. Additional Ayurvedic techniques, such as Akshi Tarpana (eye nourishment with medicated oils) for vision, Nasya (nasal drops) for respiratory health, and Abhyanga (oil massage) for tactile stimulation, further support mental clarity.
These holistic practices not only address immediate concerns but also instill lifelong habits that promote overall health and resilience. By embracing Ayurveda, adolescents can navigate the complexities of their transformative years with greater ease and balance, unlocking their full potential in a world filled with distractions and challenges.
In the age of overstimulation, Ayurveda serves as a timeless guide, offering natural solutions for mental clarity and emotional well-being. Its wisdom teaches that harmony within the body and mind is not only achievable but also essential for thriving in an increasingly chaotic world. Through Ayurveda, adolescents can find their inner calm, fostering a foundation of strength and clarity that will carry them into adulthood and beyond.
'Husband Stitch': A Medical Necessity Or Just A Tool To Objectify Women's Bodies?
Credits: AI-generated and iStock
When 36-year-old mom Angela Sanford, from Fort Mill, SC, went for an appointment for a Pap smear five years after she had her first child in 2008, her nurse midwife, who she has never seen before asked her a question she did not expect. "Who stitched you up after your first birth?"
Speaking to Healthline, Sanford shared that she just started crying when the nurse said, "This is not right." Sanford said that this was the first time she ever heard the term 'husband stitch'. Sanford was told that her stich was "too tight" by the hospitalist who managed her after her first delivery.
Also Read: US CDC Warns Of New Immune-Evasive COVID Variant In 23 Countries
“He gave you what some people call a husband stitch,” Sanford recalled the midwife telling her.
“I couldn’t connect in my mind why it would be called that. My midwife said, ‘They think that some men find it more pleasurable,’” she recalled. “My husband has been worried about me and fearful of hurting me. He would never have asked for this.”
A 'Husband Stich' - What Is It?
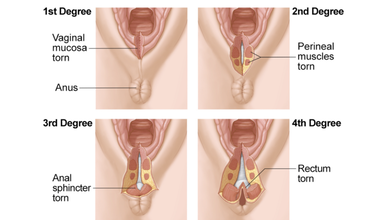
During vaginal delivery, a woman undergoes perineal tears or vaginal lacerations which means tears between the vaginal opening and anus. This causes pain, and requires stitches for grades two and higher. It also takes 4 to 6 weeks to heal. Women can experience from first to fourth degree tears.
Sometimes, a surgical incision is made in the perineum during childbirth to enlarge the vaginal opening, this is called an episiotomy. However, it is not medically necessary or a routine procedure, unless it is a case of emergency.
Stiches are required in such cases that dissolves on its own. However, a 'husband stitch', also known as "daddy stitch" is an unethical practice where an extra stitch is given during the repair process that 'tightens the vagina' to increase sexual pleasure for a male partner. While it is considered a medical malpractice, it is still done to women after vaginal delivery.
Many women face difficulty after the extra stich is given to them. In Sanford's case, she felt "excruciating" pain during sex afterwards.
Read: Romanticization And The Silent Dismissal Of Women’s Pain
When Objectifying Women's Bodies Is Made A Medical Practice
Stephanie Tillman, CNM, a certified nurse midwife at the University of Illinois at Chicago and blogger at The Feminist Midwife told Healthline: “The fact that there is even a practice called the husband stitch is a perfect example of the intersection of the objectification of women’s bodies and healthcare. As much as we try to remove the sexualization of women from appropriate obstetric care, of course the patriarchy is going to find its way in there."
Harkins, 37, said that she "kind of" laughed it off when an "old, crusty Army doctor" overstitched her so she could give her husband more pleasure. In many cases, doctors do it as a routine practice without even being told by anyone. “I couldn’t even process [it], but I kind of laughed, like what else do you do when someone says that? I had just had a baby. I didn’t think much about it because the whole birth experience was so traumatizing, but now that I think about it differently, the implications of that are just crazy.”
Episiotomy Is An Excuse For 'Husband Stitch'
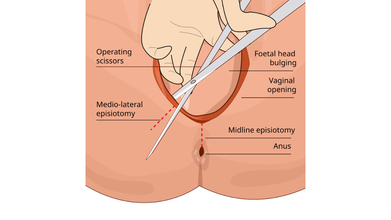
Dr Robert Barbieri, chair of obstetrics and gynecology and reproductive biology at Brigham and Women’s Hospital in Boston, told the Huffington Post that doctors were taught in the 50s and 60s that "routine episiotomy was good for women".
“What they thought is that if they did a routine episiotomy, they’d have a chance to repair it and that during the repair, they could actually create a better perineum than if they hadn’t done it. The idea [was] that we could ‘tighten things up,’” explains doctor.
However, a 2005 systematic review in the Journal of the American Medical Association found no benefit to routine episiotomy use. A 2017 Cochrane review “could not identify any benefits of routine episiotomy for the baby or the mother.” In 2016, the American College of Obstetricians and Gynecologists (ACOG) recommended that clinicians “prevent and manage” delivery lacerations through strategies like massage and warm compresses rather than making cuts on the perineum. Yet, this practice still continues inside the labor rooms.
Your Kids’ Fast-fashion Clothing May Be Laced With High Levels of Toxic Lead

Credit: iStock
While you may be buying fast-fashion clothes that are easy on your pocket and also give your children trendy looks, a new study highlights the risk of being laced with a highly toxic ingredient: lead.
The preliminary research, based on lab tests of several shirts from different retailers in the US, found that all the samples exceeded the country’s federal regulatory lead limits.
The US Consumer Product Safety Commission currently has a 100 parts per million (ppm) lead limit for children's products like toys and clothing.
"I started to see many articles about lead in clothing from fast fashion, and I realized not too many parents knew about the issue," said Kamila Deavers, principal investigator of the study, at Marian University in the US.
Deavers began the study after her young daughter’s lab reports showed elevated levels of lead in her blood from toy coatings.
How was study conducted?
The team tested 11 shirts that spanned the rainbow—red, pink, orange, yellow, gray, and blue. All brightly colored fabrics, particularly reds and yellows, showed higher levels of lead compared to more muted tones.
"We saw that the shirts we tested were all over the allowed limit for lead of 100 ppm," said Priscila Espinoza, from Marina.
The researchers explained that some manufacturers use lead (II) acetate as an inexpensive way to help dyes stick to the materials and produce bright, long-lasting color.
Children At Greater Risk
The researchers found the risk is particularly higher among younger kids as they tend to playfully suck or chew their clothes during play.
"Even briefly chewing these fabrics could expose children to dangerous lead levels,” they found in the study, to be presented at the forthcoming meeting of the American Chemical Society.
According to the US Environmental Protection Agency (EPA), lead exposure can lead to behavior problems, brain and central nervous system damage, as well as other negative health effects in children.
The agency considers children under six years old to be most at risk from exposure. Even low levels of lead in the blood of children can result in:
- Behavior and learning problems
- Lower IQ and Hyperactivity
- Slowed growth
- Hearing Problems
- Anemia
The researchers also pointed out safer alternatives to lead-based dyeing agents that already exist. These include natural and less harmful substances such as:
- Plant-based tannins (e.g., oak bark, pomegranate peel)
- Rosemary
- Alum.
Racial Discrimination Leads To Postpartum and Low Birth Weight

Credits: Canva
A recent systematic review published in the European Medical Journal found that racial discrimination leads to postpartum depression and low birth weight (LBW). Pregnant women of color were 40 per cent more likely to experience postpartum depression and have 170 per cent higher risk of delivering a baby with LBW.
The findings allowed the researchers to report that racial discrimination is a modifiable determinant of maternal and nenonatal health. Researchers also note that they should be integrated into perinatal research and care to reduce inequalities.
Large Review Examines Decades of Research
A large review of international studies has found that racial discrimination experienced by pregnant women may be linked to a higher risk of postpartum depression and poor birth outcomes, including babies born with low birth weight.
Researchers analysed nearly three decades of research that examined self reported experiences of racial discrimination among pregnant women or those who had previously been pregnant. The analysis included more than 20,300 research records and covered close to 1.5 million participants.
The study explored whether exposure to racial discrimination was associated with a range of maternal and newborn health outcomes. These included hypertensive disorders during pregnancy, gestational diabetes, mode of delivery, postpartum depression, fetal growth, gestational outcomes, infant mortality, and admission of newborns to neonatal intensive care units.
Among all the outcomes studied, the strongest link was found with postpartum depression. Women who reported experiencing racial discrimination had a 37 percent higher risk of developing postpartum depression compared with those who did not report such experiences.
Higher Risk of Low Birth Weight Among Affected Mothers
The analysis also found significant associations between racial discrimination and low birth weight in babies.
Women who experienced racial discrimination were found to have a 121 percent higher risk of delivering babies with low birth weight. The risk was even greater for very low birth weight babies, with the likelihood increasing by 170 percent.
However, researchers did not find clear links between racial discrimination and certain pregnancy complications. No strong association was observed with hypertensive disorders of pregnancy or gestational diabetes.
Findings related to preterm birth were mixed. Cohort studies did not show a clear association, while cross sectional studies suggested a modest 19 percent increased risk of premature birth among women who reported discrimination.
For several other outcomes studied, the available evidence remained inconsistent.
Stress and biological changes may explain the link
Researchers suggested that everyday experiences of racial discrimination may affect maternal health through multiple pathways.
Repeated exposure to discrimination can create chronic stress, which may affect both mental and physical health during pregnancy. The stress can also lead to social isolation and strained personal relationships, which may increase the risk of postpartum depression.
Biological changes triggered by prolonged stress may also affect pregnancy outcomes. Researchers noted that stress linked to discrimination could influence placental function, metabolism, and inflammatory responses in the body. These changes may contribute to restricted fetal growth and increase the risk of babies being born underweight.
Experts call for stronger public health response
The authors emphasized that healthcare systems should recognize racial discrimination as an important social stressor that can influence maternal and newborn health.
They recommend that routine prenatal care include screening for social stressors along with mental health assessments during pregnancy and after childbirth.
Currently, many clinical guidelines do not explicitly recognise racial discrimination as a potential risk factor for maternal and neonatal health.
Researchers say the evidence highlights the need for broader policy efforts that address discrimination at a structural level. Treating discrimination as a public health issue rather than an individual experience may help reduce health inequalities and improve outcomes for mothers and babies.
© 2024 Bennett, Coleman & Company Limited

