- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
What Are Superbugs? The Drug-Resistant Microbes Driving India’s Antibiotic Resistance Crisis

Credits: Canva
A new global study in The Lancet’s eClinicalMedicine has drawn serious concern about the sharp rise of antimicrobial resistance (AMR) in India, placing the country at the centre of what many specialists now consider a fast-moving superbug crisis. The research, titled Preprocedural screening for multidrug-resistant organisms in endoscopic retrograde cholangiopancreatography: an international, multicentre, cross-sectional observational study, shows that Indian patients had the highest worldwide rates of multidrug-resistant organisms (MDROs) among those undergoing a common endoscopic procedure.
These numbers far exceed the levels documented in Italy, the United States and the Netherlands.
What Are Superbugs?
A superbug is a strain of bacteria that no longer responds to one or more groups of antibiotics that previously worked well. This can happen through enzyme production such as carbapenemases, changes in drug targets, increased pumping out of drugs or shifts in the cell wall that block antibiotics from entering, as per National Institute of Health. When bacteria gain resistance to several antibiotic classes, the list of possible treatments becomes very small. Such resistance makes infections tougher to manage because routine medicines no longer work, leading to more severe illness.
Also Read: Ultra-Processed Food Is Harming Your Heart, Liver And Brain, Warns New Lancet Study
The recent Lancet paper used screening of patients scheduled for endoscopic retrograde cholangiopancreatography (ERCP), a frequently performed procedure, to highlight how widespread MDROs already are among Indian patients even before major interventions.
Superbugs: What Did The Lancet Study Find?
The study assessed more than 1,200 patients across India, Italy, the Netherlands and the United States. Among them, 83.1 per cent of Indian patients carried at least one superbug, a figure far higher than those in the other countries.
- Italy: 31.5 per cent
- United States: 20.1 per cent
- Netherlands: 10.8 per cent
Which Superbugs Are The Biggest Culprits In India?
A few resistant pathogens account for most of the problem in the country, as per The Lancet Study:
Also Read: The Kessler Twins Die By Assisted Suicide in Germany; How It Differs From Euthanasia
Enterobacterales, especially Klebsiella pneumoniae and Escherichia coli: These cause a large share of urinary tract infections, bloodstream infections and hospital-related illnesses. The study noted that nearly 70.2 per cent of Indian patients carried ESBL-producing strains.
Carbapenem-resistant Gram-negatives (CRGNs): India’s carbapenem-resistance rate for key pathogens was around 23.5 per cent, signalling that even some last-resort drugs fail against these infections.
Acinetobacter baumannii and Pseudomonas aeruginosa: These are common in intensive care units, often highly resistant and linked with ventilator-associated pneumonia. Surveillance in India shows very high resistance levels in both.
Staphylococcus aureus (MRSA, or methicillin-resistant Staph. aureus): This remains an established cause of surgical site and hospital-acquired infections.
Together, these organisms form part of the “ESKAPE” group (Enterococcus, Staph. aureus, Klebsiella, Acinetobacter, Pseudomonas and Enterobacter), which represents the central challenge in antibiotic resistance. India’s unusually high carriage and infection rates of these pathogens increase the threat both in hospitals and in the community, as highlighted in The Lancet study.
Resistance may be inevitable, yet it can still be controlled. The new findings make it clear that India cannot afford further delays. Antibiotic resistance is no longer a niche concern. With such high carriage levels, every hospital visit becomes a potential source of spread and every procedure carries added risk. Officials often speak about “containing resistance,” but the timeframe to act is shrinking. Without stronger antibiotic stewardship, timely diagnostics and firm infection-control practices, the country may lose access to many dependable first-line antibiotics for everyday infections, undoing years of medical progress.
Tamil Nadu Increases Preventative Chickenpox Measures As Cases Rise
Credit: Canva
Tamil Nadu health authorities have ramped up surveillance efforts and implemented preventive and control measures to curb rising chickenpox cases in the state.
The Directorate of Public Health (DPH) and Preventive Medicine has instructed all health officers to intensify active and passive surveillance in all government and private health facilities, schools, colleges and hostels.
They were also directed to ensure that all suspected and confirmed cases are entered into the Integrated Disease Surveillance Programme (IDSP) line list with complete demographic and clinical details.
All medical officers across the state have further been asked to be alert to differentiate chickenpox from other rash illnesses such as measles, rubella, and hand, foot and mouth disease.
This comes weeks after doctors across Pune also warned against the exponential rise in chickenpox cases this winter.
Dr Shirish Kankariya, head of paediatrics at Apollo Hospital Swargate, said he had seen around 15 chickenpox patients in Jan alone, and the current season has brought a visible uptick in cases.
"Chickenpox cases have risen. We are also seeing infections in older children and adult family members, who never had the disease earlier," he told Times of India.
Dr Prateek Kataria, consultant pediatrician and neonatologist at Sahyadri Hospital also noted that out-patient departments (OPDs) have recently seen a large increase confirmed chickenpox cases this year.
He also told the publication: "We are seeing many children with chickenpox in the OPD even among those who have taken both doses of the vaccine. This is expected because the vaccine does not guarantee 100% protection, but vaccinated children usually develop milder illness and do not need hospitalization."
What Is Chickenpox And How Does It Spread?
Chickenpox, caused by the varicella-zoster virus, is extremely contagious and spreads through respiratory droplets or direct contact with someone who is infected. In children, it often starts as a mild rash accompanied by fever, but it can spread quickly in crowded areas.
The virus can also be transmitted through coughing or sneezing, and it is most infectious a day or two before the rash appears and in the early days of the rash. In individuals with weak immunity, the dormant virus may reactivate later in life, causing shingles (herpes zoster).
How To Detect Chickenpox Symptoms Early?
Spotting chickenpox early means looking for general warning signs like fever, fatigue, headache, and loss of appetite, which usually appear one to two days before the rash.
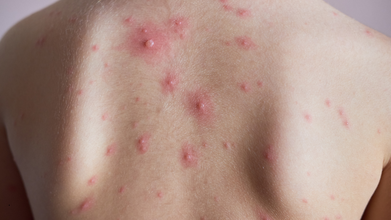
The rash itself starts as tiny red spots that later form fluid-filled blisters and eventually scab over. Paying attention to these early symptoms, especially after known exposure, can help identify the infection sooner.
How To Spot A Chickenpox Rash
The first rash usually shows up as small red bumps on the face, chest, or back. These bumps quickly turn into blisters filled with fluid, which are contagious. Over a few days, the blisters break and crust over, forming scabs. It’s common to see spots, blisters, and scabs all at the same time, according to the CDC.
Stages Of Chickenpox
The Mayo Clinic explains that chickenpox progresses in three main stages:
- Incubation Stage (10–21 days): After exposure, the virus remains inactive. Infected individuals typically show no symptoms during this period.
- Prodromal Stage (1–2 days): Early signs include fever, tiredness, headache, loss of appetite, and body aches. This is also when the virus can start spreading to others.
- Rash Stage (5–10 days): Red, itchy spots appear first on the face and chest, spreading across the body. These spots develop into fluid-filled blisters that scab over within a few days. Mild fever, itching, and discomfort are common during this stage.
Breast Cancer To Reach Over 3.5 Mn By 2050, Deaths To Surge 44% Predicts Lancet Study

Credit: Canva
A new study published in The Lancet Oncology journal today revealed that breast cancer continues to be the most common cancer among women worldwide, and predicted that the number of new cases of the deadly disease will reach more than 3.5 million globally in 2050 -- rising by a third from 2.3 million in 2023.
The Global Burden of Disease analysis with data from 204 countries revealed that despite advancements in breast cancer treatments, yearly deaths from the disease will rise by 44 percent -- from around 764,000 to 1.4 million.
While breast cancer disproportionately impacts countries with limited resources, maintaining a healthy lifestyle, including not smoking, getting sufficient physical activity, lowering red meat consumption, and having a healthy weight were found to prevent over a quarter of healthy years lost to illness and premature death.
“Breast cancer continues to take a profound toll on women’s lives and communities,” said lead author Kayleigh Bhangdia from the Institute for Health Metrics and Evaluation (IHME), University of Washington, US.
“While those in high-income countries typically benefit from screening and more timely diagnosis and comprehensive treatment strategies, the mounting burden of breast cancer is shifting to low- and lower middle-income countries where individuals often face later-stage diagnosis, more limited access to quality care, and higher death rates that are threatening to eclipse progress in women’s health,” Bhangdia added.
Inequalities In Breast Cancer Burden
The study revealed that the rates of new cases remain highest in high-income countries (HICs), but are growing fastest in low-income countries (LICs).
Women in low- and lower-middle-income countries accounted for 27 percent (around 628,000) of new cases globally, exposing likely disparities in timely diagnosis and shortages of quality treatment, including radiotherapy machines, chemotherapy drugs, and pathology labs, and standard treatments.
In 2023, an estimated 2.3 million new breast cancers were diagnosed worldwide in women (with 73 percent or 1.67 million cases occurring in high- and upper-middle-income countries). Of these, 764,000 ended in deaths (with 39 percent or 300,000 deaths occurring in low- and lower-middle-income countries).
Further, the number of years of healthy life lost due to poor health and early death more than doubled from 11.7 million years in 1990 to 24 million years in 2023.
Women in low- and lower-middle-income countries also contribute to more than 45 percent of all the ill-health and early deaths from breast cancer globally (nearly 11 million years of healthy life lost).
Three-fold Rise In Pre-menopausal Breast Cancer
The study reported a three-fold rise in pre-menopausal breast cancer in women aged 55 or older in 2023 -- compared to women aged 20-54 years.
However, rates of new cases have risen in women aged 20-54 years (up 29 percent) since 1990, with rates in older women remaining relatively unchanged.
Major Lifestyle Risk Factors
In 2023, 28 percent of the global breast cancer burden (6.8 million years of healthy life lost to disability, illness, and early death) was linked to six potentially modifiable risk factors. These include:
- High red meat consumption -- linked to nearly 11 percent of all healthy life lost
- tobacco use (including second-hand smoke; 8 percent),
- high blood sugar (6 percent),
- high body mass index (4 percent),
- high alcohol use and low physical activity (both 2 percent)
Substantial progress has been made in reducing the global breast cancer burden linked to high alcohol use and tobacco between 1990 and 2023, which declined by 47 percent and 28 percent, respectively.
Donald Trump's Neck Appears To Have Redness And Rashes, White House Says A Skin Cream Caused It
Credits: AP
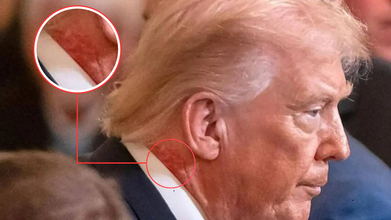
Donald Trump is again in the news, this time not for his cognitive conditions and speculations around it, but for a skin rash and redness around his neck. During a Medal of Honor ceremony in the East Room of the White House, many pointed out the redness around his neck and asked if there was any underlying medical reason to it. The close-up photos shows clear red marks around the 79-year-old president's neck.
Also Read: Breast Cancer To Reach Over 3.5 Mn By 2050, Deaths To Surge 44% Predicts Lancet Study
Why Does President Trump Have Red Rashes Around His Neck?
As per the White House, this redness around his neck is due to a skin cream he has been using. However, the White House has not given any specific reason behind the treatment for which the skin cream has been prescribed. "President Trump is using a very common cream on the right side of his neck, which is a preventative skin treatment, prescribed by the White House Doctor,” Sean Barbabella, the president's doctor, said in a statement. “The President is using this treatment for one week, and the redness is expected to last for a few weeks.”
No follow-up questions on the treatment were given, neither any clarity was given on the condition. However, zoomed in photos from as far back as the Board of Peace meeting at the US Institute of Peace on February 19 too show the redness on President's neck.
Topical treatments can sometimes lead to temporary skin irritation, flushing, or redness - especially if they contain active ingredients like retinoids, benzoyl peroxide, alpha hydroxy acids, or prescription-strength dermatological compounds.
Trump’s medical report from his April 2025 physical exams has noted he was on mometasone cream “as needed” for an unspecified skin condition.
Also Read: Ashley Dalton Diagnosed With Incurable Breast Cancer Stands Down From Her Position
Why Do Skin Cream Cause Redness And Rashes?
While this is not true for all creams, some skin cream could make your skin red by increasing the turnover of cells that stimulate collagen production or reduce inflammation.
In this process, the skin may appear red, slightly inflamed, or sensitive – especially in areas like the neck, which tends to have thinner skin than the face.
Common reasons for redness caused by skin cream include:
- Irritant contact dermatitis
- Allergic reaction to ingredients
- Increased blood flow from active compounds
- Over-application of product
- Sun sensitivity after use
- Skin around your neck may especially react more visibly than other areas due to its delicate texture.
When should redness be a concern?
Even though temporary redness from skincare products is usually harmless, doctors say you must always use creams after a prescription and reach out to them in case of:
- Severe burning or itching
- Blistering or peeling
- Swelling of the face or throat
- Symptoms lasting more than a few days
- Signs of infection
- In most cases, discontinuing the product allows the skin to return to normal within a short period.
© 2024 Bennett, Coleman & Company Limited

