- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
The Right Approach To Manage Endometriosis
Living with endometriosis can be a daily battle, from dealing with intense pain to managing social and work-life disruptions. While conditions like PCOS don’t directly cause endometriosis, both often coexist and share challenges that impact physical, emotional, and mental health.
However, when healthcare providers overlook these complexities and focus on weight shaming, patients are less likely to seek help, worsening their condition.
Here’s how one can look into managing endometriosis, its relationship with PCOS, and how a compassionate healthcare approach can make a difference.
Understanding Endometriosis and Common Symptoms
Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus, causing pain and other symptoms. According to Dr Anuradha Kapur, Principal Director (Obstetrics & Gynecology) & Head of Unit at Max Smart Super Speciality Hospital, Saket, symptoms can vary widely: “Many experience painful periods, pain during intercourse, bloating, and fatigue. Others may have irregular bleeding, pain during bowel movements, and even asymptomatic cases,” she notes. Endometriosis is complex and can be difficult to diagnose, especially in asymptomatic cases or when symptoms overlap with other conditions like PCOS.
How Endometriosis Affects Daily Life
Endometriosis can disrupt daily routines, impacting work and relationships due to fatigue and persistent pain. Dr Sonam Simpatwar, a reproductive medicine specialist at Central Railway Hospital, Byculla, Mumbai, highlights the importance of staying alert to symptoms, especially for those with risk factors like family history or high estrogen levels. “Symptoms can be subtle, and many women may not experience severe signs until they face issues like infertility,” she explains.
For some, managing endometriosis involves lifestyle changes, pain management, and treatments ranging from hormonal therapies to surgical options. Regular gynaecological check-ups are crucial for catching signs early and avoiding long-term complications.
The PCOS and Endometriosis Connection: What’s the Link?
PCOS, or Polycystic Ovary Syndrome, is often confused with endometriosis due to some overlapping symptoms like irregular periods.
However, as Dr. Kapur explains, “PCOS doesn’t cause endometriosis. They are distinct conditions with different causes—PCOS results from hormonal imbalances, while endometriosis involves abnormal tissue growth outside the uterus.”
Although they don’t directly cause one another, patients with both conditions face unique challenges, including a higher risk of infertility, irregular cycles, and persistent pain.
Managing PCOS can be equally challenging, particularly because it’s closely tied to insulin resistance and weight. Lifestyle changes, such as a balanced diet and regular exercise, are often recommended, but these suggestions can sometimes become oversimplified, leaving patients feeling body-shamed or unsupported.
Addressing the Weight-Shaming Issue in Healthcare
Many patients with PCOS and endometriosis express discomfort in seeking medical help due to a tendency among some doctors to focus heavily on weight, often without offering practical support. Patients report feeling judged or dismissed, leading many to avoid seeking the care they need.
Dr Kapur highlights that while “weight can impact insulin resistance and hormone levels in PCOS, it’s crucial for doctors to adopt an empathetic approach.” This approach means understanding the complexities of the condition rather than simply prescribing weight loss.
For instance, doctors might shift the conversation from weight alone to include lifestyle guidance that patients can realistically adopt. Suggesting a referral to a nutritionist or creating a structured plan can be more supportive, focusing on the patient’s overall health and making them feel seen beyond their weight.
According to Dr Simpatwar, “PCOS already carries mental and emotional burdens, and weight shaming only exacerbates feelings of isolation.” Such experiences can discourage individuals from seeking the medical attention they need, creating a barrier to effective care.
Breaking the Weight-Stigma Cycle in Patient Care
A supportive doctor-patient relationship can be transformational in managing PCOS and endometriosis effectively. Dr Simpatwar suggests, “Doctors should focus on creating an open dialogue, discussing how diet and exercise can positively impact symptoms without emphasizing weight as the only solution.”
When patients feel heard and understood, they’re more likely to actively engage in their health journey. Here are some ways doctors can offer compassionate support:
Focus on Health, Not Just Weight: Emphasising improved energy levels and reduced symptoms over numbers on a scale can help patients feel more positive and proactive.
Personalised, Empathetic Language: Instead of “You need to lose weight,” language like, “Let’s work together on symptom management through small, realistic changes” feels more encouraging.
Holistic Approaches and Counseling Referrals: Some patients benefit from mental health support due to the emotional toll of chronic pain and hormonal changes, which many patients appreciate when offered.
Practical Tips for Managing Endometriosis and PCOS
While every individual’s experience is unique, there are practical strategies to manage life with endometriosis and PCOS that focus on overall well-being rather than just weight.
Focus on Diet and Nutrition: Incorporate anti-inflammatory foods, like leafy greens and fatty fish, and reduce refined sugars. A balanced, low-GI diet can aid with insulin resistance and improve energy levels.
Exercise Regularly for Symptom Relief: Low-impact exercises like yoga, swimming, and walking can help alleviate pain and reduce stress, benefiting both endometriosis and PCOS symptoms.
Build a Support Network: Connecting with others who have similar experiences can provide emotional relief and motivation, helping you feel less isolated.
Communicate Openly with Healthcare Providers: Finding a healthcare provider who listens and validates your concerns can make a big difference. If you feel unheard, don’t hesitate to seek a second opinion.
Consider Hormonal and Non-Hormonal Treatments: Options like hormonal therapy or alternative birth control can manage symptoms; consult your doctor to find what works best for you.
Why Many Older Men Struggle to Conceive Despite ‘Good Health’

Chronic stress can take a toll on sperm count. (Photo credit: iStock)
Many men believe that as long as they feel healthy, active, and free from major illness, their fertility remains intact. While men do not have a sudden fertility cut-off like women, age still plays an important role when it comes to male fertility. Currently, a large number of men wish to start families later in life, often thinking their good health guarantees easy conception and fatherhood. They often neglect the age factor, even though it is linked to hormonal imbalance, stress, and genetic issues. A large number of men are unaware of their fertility health and continue to suffer. However, even in the absence of visible health problems, older men may face unexpected fertility challenges. Dr Madhukar J Shinde, Fertility Specialist at Nova IVF Fertility, PCMC, Pune, answered this for Health and Me.
Read more: The Overlooked Role of Men in IVF: Why Their Silent Strength Is Key to Fertility Success
Why do older men struggle with infertility?
Decline in sperm quality: Various studies have confirmed that as men age, sperm count, movement, and shape can slowly decline. Even if the numbers appear normal, DNA damage in sperm increases with age, which can reduce the chances of successful fertilisation.
- Hormonal imbalance: It is important to note that testosterone levels naturally decrease over time. Lower testosterone can affect sperm production, sexual function, and overall reproductive performance, even when a man feels physically fit.
- Some medical conditions tend to take a toll on fertility: Conditions such as diabetes, high blood pressure, and thyroid disorders become more common with age. These may be well-managed and symptom-free, but can still affect sperm health and fertility.
- Stress and other lifestyle factors can impact fertility: Chronic stress, lack of sleep, smoking, alcohol consumption, or exposure to pollution can take a toll on sperm quality and lead to fertility issues that can be worrisome for men. Preservatives in a lot of frozen and junk food not only contribute to poor fertility health, but research suggests they may also affect DNA function. Therefore, men should stay vigilant.
- Genetic issues: Advanced paternal age is associated with a higher risk of genetic mutations in sperm. This can further affect embryo development and increase the risk of miscarriage or certain developmental conditions.
Men must stay in touch with a fertility consultant who can design an appropriate treatment plan. The expert will evaluate them thoroughly and suggest lifestyle modifications such as a well-balanced diet, exercise, stress management through meditation, and medication for conditions such as diabetes, hypertension, and cholesterol. Awareness helps men take informed steps towards parenthood, even later in life. Certain pre-medications, including antioxidants advised by a fertility consultant, may significantly help in reducing DNA fragmentation, which contributes to poor sperm function. Therefore, men should prioritise their reproductive health, stay informed, and not suffer in silence.
High BP? This Ancient Chinese Practice May Be As Good As Brisk Walking

Credit: iStock
High blood pressure (BP) has become a public health problem that is driving cardiovascular diseases like heart attacks and strokes globally. While medications are important to keep hypertension under control, lifestyle changes and healthy practices are also crucial.
Several global health guidelines recommend regular physical activity, but adhering to exercise programs daily becomes a challenge for many people. But in the overtly busy schedules, sparing 10 minutes for an exercise regimen can be easier than travelling to the gym.
A large randomized clinical trial, published in the Journal of the American College of Cardiology (JACC), has proved that a traditional Chinese mind-body practice — baduanjin — may help lower blood pressure, that too, without any equipment.
Baduanjin is a slow, structured movement, focused on deep breathing and meditation.
Importantly, the clinical trial proved that the ancient Chinese technique could lower BP as effectively as brisk walking.
In people practicing baduanjin, BP reductions were seen after three months and were sustained for one year.
"Given its simplicity, safety, and ease with which one can maintain long-term adherence, baduanjin can be implemented as an effective, accessible, and scalable lifestyle intervention for individuals trying to reduce their blood pressure," said Jing Li, Director, National Center for Cardiovascular Diseases in Beijing, China.
Baduanjin: The 10 Minute Routine
Baduanjin is a standardized eight-movement sequence that integrates aerobic, isometric, flexibility, and mind-body components.
It has been in practice for centuries and commonly performed in community settings across China. The routine typically takes 10–15 minutes and requires no equipment and only minimal initial instruction.
Because it is low- to moderate-intensity, it is considered safe and accessible for many adults.
Also read: Cardiovascular Diseases Lead As India’s Top Killer: US Cardiologist Points Out Risk Factors
The Clinical Trial
A team of Chinese researchers led the first large, multicenter randomized trial to look at the impact of baduanjin on blood pressure.
They followed 216 participants, aged 40 years or older, across seven communities to determine changes in 24-hour systolic BP from baseline to 12 and 52 weeks.
Compared to people indulging in self-directed exercise, practicing baduanjin five days a week reduced
- systolic blood pressure by approximately 3 mg Hg
- systolic blood pressure by 5 mg Hg.
Notably, the benefits were sustained even without ongoing monitoring, a key challenge for many lifestyle interventions that struggle to maintain long-term adherence outside structured programs.
"Baduanjin has been practiced in China for over 800 years, and this study demonstrates how ancient, accessible, low-cost
approaches can be validated through high-quality randomized research," said Harlan M. Krumholz, Editor-in-Chief of JACC and the Harold H. Hines, Jr Professor at the Yale School of Medicine.
"The blood pressure effect size is similar to that seen in landmark drug trials, but achieved without medication, cost, or side effects. This makes it highly scalable for community-based prevention, including in resource-limited settings," they added.
Also read: AHA Cholesterol Guidelines 2026: How Indians Can Improve Heart Health
How To Practice Baduanjin
- Stand upright with your feet shoulder-width apart and keep your movements slow and controlled.
- Coordinate each motion with steady, deep breathing, inhaling and exhaling smoothly as you move.
- Move through the traditional eight postures in sequence, focusing on posture, balance, and relaxation rather than speed or force.
- Practice for about 10 to 15 minutes a day in a quiet space, maintaining calm attention throughout.
Endometriosis In Working Women: Gynaecologist Says Yoga, Stress Management Can Help

Long working and sitting hours can worsen endometriosis in women. (Photo credit: AI generated)
Are you a working professional? Have you been diagnosed with endometriosis? Worried about how this condition can impact your career? Well, don’t panic! We give you vital tips to manage the symptoms of endometriosis without compromising your professional aspirations. Dr. Kanika Gera Thakral, Consultant – Obstetrics & Gynaecology, Motherhood Hospitals, Greater Noida, spoke about the effects of endometriosis on working women and what women can do to not let the pain take a toll on their work life.
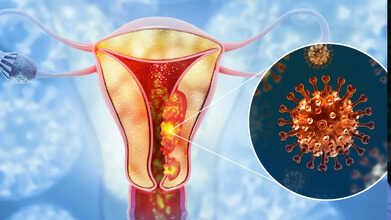
What is endometriosis?
Endometriosis happens when tissue similar to the lining of the uterus grows outside the uterus. These tissues commonly develop on the ovaries, fallopian tubes, or the pelvic lining. Endometriosis affects many women and can impact their daily lives, including their ability to work comfortably. Many women continue their professional responsibilities despite experiencing severe discomfort, fatigue, and pain.
Raising awareness about the condition and encouraging supportive workplaces can help women manage both their health and career more effectively. Since it is a progressive disorder, timely intervention remains key to managing it. In many cases, women live with symptoms for several years before receiving the correct diagnosis, which can delay treatment and affect their quality of life.
Read more: The Right Approach To Manage Endometriosis
The workplace challenge
Many working women who are diagnosed with endometriosis tend to experience symptoms such as pelvic pain, cramps, fatigue, nausea, and heavy menstrual cycles. These symptoms can make it difficult to maintain productivity at work, especially during flare-ups. Hence, women will be unable to concentrate on work or finish the tasks. Some may miss deadlines and meetings due to the painful symptoms. Women will have to skip going to work when the symptoms are intense and will have to rest at home. So, women living with endometriosis may face interruptions in their career growth and reduced working hours. But don’t worry, it is possible to manage this condition and give your best at work.
- Long working hours, prolonged sitting, workplace stress, irregular meals, and lack of adequate rest can sometimes worsen symptoms of endometriosis.
- Apart from physical discomfort, the condition can also affect emotional well-being. Living with chronic pain may lead to stress, anxiety, or frustration, which can indirectly impact workplace confidence and productivity.
Strategies for managing work and endometriosis
It is necessary for women with endometriosis to go for regular check-ups and follow-ups with the doctor. Women can continue to pursue their professional goals by adopting practical strategies to manage the condition. Open communication with employers when it comes to flexible schedules can help overcome stress and anxiety. Women should have access to remote working to avoid unnecessary travel due to pain.
The work-from-home option can be given to the women when needed by them. Planning demanding tasks during times of higher energy and maintaining a balanced daily routine can also improve productivity at work. Women should make sure to keep essential medications, a heating pad, or comfort aids at their desk to be able to relieve sudden discomfort. Likewise, using ergonomic seating or maintaining good posture while working may reduce pelvic and even back discomfort. Women should also connect to support groups that help to provide emotional reassurance and useful coping strategies that include yoga and meditation.
Lifestyle habits also play an important role. Regular physical activity, adequate sleep, stress-management techniques such as yoga or meditation, and following an anti-inflammatory diet rich in fruits, vegetables, whole grains, and healthy fats may help reduce flare-ups.
Read more: Women With Endometriosis Are Earning Less, Reveals Study
Treating endometriosis
Treatment is particularly based on the severity of symptoms. Women will be advised lifestyle modifications such as regular exercise, stress management, and an anti-inflammatory diet. Non-steroidal anti-inflammatory drugs may help reduce discomfort. Hormonal therapies may also be used to control symptoms. Some women will be advised to undergo laparoscopy to remove endometriotic cysts. Minimally invasive surgery can help remove lesions and restore pelvic anatomy, which may also improve fertility in some cases. In advanced cases, surgery can be recommended to women.
With timely care and supportive workplaces, women can pursue their ambitions without letting endometriosis interfere with their careers.
© 2024 Bennett, Coleman & Company Limited

