- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Why Is There A Rise In Testosterone Prescriptions In UK?
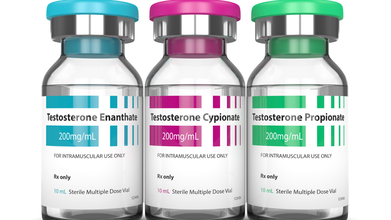
Credits: iStock
Testosterone prescription in the UK have surged in recent years. Reels and TikTok videos with medical practitioner talking about testosterone shots, how to take it, and the do's and dont's are easily found on social media platform. Many doctors, patients and private clinics are debating on whether the hormone is genuine treatment for low libido or just a wellness trend.
As per the NHS Business Authority data compiled by the Care Quality Commission and reported by the BBC, testosterone prescriptions increased by 135 per cent between 2021 and 2024. This spike comes when people in Britain are also having less sex than the previous generation, noted a BBC report. This has raised an important question. Are hormones the missing link or are there deeper social changes at play?
Hormone Therapy: Is It Need Of The Hour?
In the 1990s, Alan Reeves performed in front of thousands as part of the male dance troupe Dreamboys and even appeared in the Spice Girls film Spice World. But in his thirties, his energy dipped and his libido faded.
“I just didn't feel right,” Reeves told the BBC.
Now 52 and working as a fitness and lifestyle coach in London, he began testosterone replacement therapy, or TRT, and says the difference was dramatic. He described feeling transformed from “a grumpy old man” to someone who felt decades younger.
His relationship had been struggling before treatment. “We were going without sex for three, four months at a time. I just wasn't interested,” he said in the BBC report, adding that such changes can damage relationships.
Women are increasingly seeking treatment too. Menopause blogger Rachel Mason told the BBC the hormone was “amazing” for her concentration, energy and libido.
Sex Drive Is Fading In Britain
There is a broader trend in the rise of prescribed testosterone. The long running National Surveys of Sexual Attitudes and Lifestyles documented a steady decline in sexual frequency over decades. People aged 16 to 44 reported sex about five times a month in 1990, by 2010, the number had dropped to three times. Researchers further predict a downward trend to continue.
Soazing Clifton, academic director of the survey, told the BBC that the fall appears across almost every demographic, including couples living together.
“No data we have so far can really tell us with any confidence why, as a population, we are no longer having sex as much,” she said.
Experts point to multiple factors. GP and sex therapist Dr Ben Davis said modern pressures play a role. Stress, loneliness, depression and constant digital distraction all reduce desire.
Another explanation is biological. Consultant urologist Professor Geoffrey Hackett told the BBC testosterone levels in men are declining, partly linked to obesity, diabetes and sedentary lifestyles. Lower hormone levels increase the likelihood of low libido, though not everyone with low testosterone experiences sexual problems.
For some patients, the results feel life changing.
Melissa Green, 43, said the treatment “gave me my life back” and improved both energy and intimacy in her marriage after she sought help from a private clinic, according to the BBC.
But not everyone benefits. Cheryl O’Malley stopped taking testosterone after a year due to intense anger and excessive sexual arousal. “I felt out of control,” she said in the BBC report.
Doctors note that side effects can include acne, hair growth and weight gain in women, and mood swings, infertility and prolonged erections in men.
A Boom In Private Industry
The growing demand has fuelled a booming private clinic market. Some NHS clinicians are concerned.
Dr Paula Briggs described it to the BBC as a “gravy train”, saying patients may pay for treatments they do not need and warning that advertising has “blown everything out of proportion”.
Private providers disagree. GP Jeff Foster told the BBC the private sector is filling a care gap because the NHS lacks capacity to diagnose large numbers of men who may have low testosterone.
Guidelines also differ. Some professional bodies recommend treatment below 12 nmol per litre while NHS thresholds can be lower, leading some patients to seek private prescriptions after being refused treatment publicly.
Despite its popularity, doctors caution that TRT is not a universal fix.
“For some, medication can be really transformative,” Davis told the BBC. “But there are so many factors that play into a low libido and testosterone is not the only answer.”
Even Reeves agrees. After seven years on therapy, he says lifestyle changes matter just as much.
Otherwise, he said, taking testosterone alone is like installing a Ferrari engine in a worn out car.
As prescriptions continue to rise, the debate reflects a broader question about modern health. Is declining desire a medical problem, a social shift, or a mix of both? The answer may determine whether testosterone therapy becomes mainstream medicine or remains a controversial shortcut to vitality.
Why Hemophilia Care in India Lags Behind Globally, Expert Reveals: World Hemophilia Day
Credit: Canva
Hemophilia is a rare genetic bleeding disorder, usually inherited, wherein blood cannot clot properly due to low levels of clotting factors, causing prolonged bleeding or spontaneous internal hemorrhages.
Symptoms include easy bruising, joint pain/swelling, and excessive bleeding. While not curable, it is treated with factor replacement therapy and gene therapy.
India has the world's second-largest population of hemophilia patients, with estimates suggesting over 70,000 to over 1,36,000 cases of Hemophilia A and B. However, while around 13,000 to 19,000+ patients are registered, many remain undiagnosed.
This World Hemophilia Day, Dr Dr Bilal Ahmed, Prof and Head, Government Medical College, J&K exclusively told Healthandme that the primary reason why thousands of Indians remain undiagnosed and unable to access proper care is due to budget constraints, lack of awareness among policymakers, and the need for technocrats to advocate boldly for regular replacement therapy.
Despite having the second-largest hemophilia population, only 9-10 percent receive treatment as compared to 80-100 percent in some European countries.
The expert explained: "Money plays an important role. Every center in India has, at their own level, their own policymakers and the people who are at the helm of affairs. We are the second home for the hemophilia and we can change the lives of these people by having the regular replacement but it is all depending upon the perception of individual centers."
He also noted that the government needed to introduce policy reforms endorsing regular replacement therapy as the gold standard to help ensure equitable access to patients.
The median age at diagnosis for severe hemophilia in India stands at 60 months—five full years—compared to under 12 months in high-income countries. This delay is not just a matter of time but one that poses a risk of serious clinical consequences. Late diagnosis often means repeated, unmanaged bleeding episodes during early childhood, particularly into joints, before appropriate treatment begins.
Early Warning Signs
The three types of this condition include :
- Hemophilia A: This is the most common type. You may develop this condition because you have low levels of clotting factor 8 (factor VIII).
- Hemophilia B: You may have this type if you don’t have enough clotting factor 9 (factor IX).
- Hemophilia C: Hemophilia C is also known as factor 11 (factor XI) deficiency. It’s the least common type of hemophilia.
- Bleeding into the joints. This can cause swelling and pain or tightness in the joints. It often affects the knees, elbows, and ankles.
- Bleeding into the skin (which is bruising).
- Bleeding into the muscle and soft tissue, which can cause a build-up of blood in the area (called a hematoma).
- Bleeding of the mouth and gums, including bleeding that is hard to stop after you lose a tooth.
- Bleeding after circumcision.
- Bleeding after having shots, such as vaccinations.
- Bleeding in the head of an infant after a difficult delivery.
- Blood in the urine or stool.
- Frequent and hard-to-stop nosebleeds.
Treatment Options
The treatments for haemophilia have never been more effective, but they work only for patients who have been diagnosed. In a condition where every missed bleed moves a joint closer to permanent damage, the most important clinical act is also the most basic one: recognition.
The main treatment for severe hemophilia involves replacing the clotting factor you need through a tube in a vein. This replacement therapy can be given to treat a bleeding episode in progress. It can also be given on a regular schedule at home to help prevent bleeding episodes. Some people receive continuous replacement therapy.
Replacement clotting factor can be made from donated blood. Similar products, called recombinant clotting factors, are made in a laboratory, not from human blood.
Second Chances: What to Do After an Unsuccessful IVF Attempt
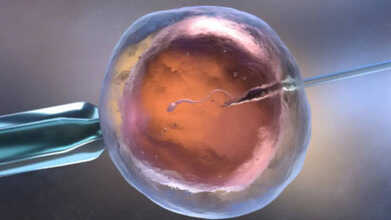
IVF can be helpful for patients battling infertility. (Photo credit: iStock)
Failure to conceive using IVF can be devastating, but one should realise that one failed attempt does not determine a couple’s fertility journey. The success of IVF is determined by various factors such as age, egg and sperm quality, and the uterine environment, as well as underlying medical conditions. An unsuccessful attempt can also be a valuable source of clinical information that can be used to guide future treatment procedures. It should be seen not as an ending but as a starting point for more individualised and effective care in future cycles.
What happens after an unsuccessful IVF attempt?
It is necessary to conduct a careful assessment after an unsuccessful IVF cycle. This involves a review of the stimulation protocol, the response of the ovaries, the quality of the retrieved eggs, fertilisation rates, and embryo growth. In some instances, issues with embryo quality, implantation, or hormonal imbalances may be identified. Further tests such as genetic testing of embryos, evaluation of the receptivity of the uterine lining, or screening for conditions such as endometriosis or thyroid disorders may be recommended. These insights can be used to make the subsequent cycle more precise.
Mental health
Emotional health is highly significant in the healing process. A failed IVF cycle may have a considerable psychological impact, leading to stress, anxiety, and self-doubt. Such feelings should not be disregarded, and appropriate support should be sought, whether through counselling, support groups, or simply by talking to a partner. Addressing emotional health not only aids coping but also has a beneficial effect on overall treatment outcomes.
Lifestyle changes to make
Lifestyle changes can also play a role in improving outcomes in future attempts. Maintaining a healthy weight, following a balanced diet, managing stress, and avoiding smoking or excessive alcohol consumption are important factors. Hormonal balance and reproductive health may also be supported through adequate sleep and moderate exercise. Small yet consistent lifestyle adjustments may help prepare the body for another cycle.
Treatment options
Treatment plans can be modified based on previous results. This might include changes in medication regimens or the use of advanced procedures such as intracytoplasmic sperm injection (ICSI), assisted hatching, or preimplantation genetic testing (PGT). In some instances, the use of donor eggs or sperm, or options such as frozen embryo transfer, may be considered. All approaches are personalised, taking into account the medical history of the couple and their previous response to treatment.
How to time the next IVF attempt properly?
The timing of the next attempt is another important aspect. While some individuals may be physically ready to proceed soon after a failed cycle, others may benefit from taking time to rest and recover both physically and emotionally. Such a break also allows for further evaluation and optimisation of health parameters before resuming treatment.
In the end, persistence combined with a personalised, evidence-based approach tends to increase the likelihood of success. Advancements in reproductive medicine continue to offer new hope, even after setbacks in IVF. With careful assessment, emotional support, and appropriate adjustments in treatment, many couples achieve successful pregnancies in subsequent cycles.
Family Planning Done Right: IVF Expert's Tips To Improve Embryo Quality

Consult with an expert before planning a pregnancy to rule out the possibility of infertility. (Photo credit: iStock)
Women, are you planning a pregnancy? Do you wish to fulfil the dream of motherhood? Did you know it is possible to improve embryo quality for successful conception? Do not worry—we have you covered. This article highlights how appropriate lifestyle choices, proper nutrition, and timely medical care can play a key role in improving embryo quality. Hence, it is essential to follow the guidelines given below.
Also Read: Breast Cancer Screening: AI May Predict Tumours Before Mammograms Can Detect Them
Why is Infertility a common concern now?
Dr Jyoti Gupta, Senior IVF Consultant, Motherhood Hospitals, Gurgaon, in an interview with Health and Me, shared some simple tips for couples. These can go a long way in improving embryo quality and may even enhance the chances of conception.
Currently, many couples are battling infertility and undergoing in vitro fertilisation (IVF). Embryo quality is one of the most important factors influencing the success of pregnancy, especially in couples who have opted for IVF. Good-quality embryos have a higher likelihood of implantation, resulting in a healthy and successful pregnancy. Even though some factors, such as age and genetics, cannot be changed, there are several ways to support and improve embryo quality both naturally and medically.
Embryo quality is based on the health of both the egg and sperm. As women age, egg quality tends to decline, which can affect embryo development. Moreover, sperm health also plays a vital role. Lifestyle, diet, and stress can negatively impact egg and sperm quality and, in turn, embryo quality.
Tips to improve embryo quality
It is necessary for couples to focus on their diet to improve embryo quality. Including foods rich in antioxidants, such as fresh fruits, vegetables, nuts, and seeds, can help protect eggs and sperm from damage. Nutrients such as folic acid, omega-3 fatty acids, vitamin D, and iron are important for reproductive health. It is also important to stay well hydrated and cut down on processed foods, excess sugar, and caffeine. Seek expert guidance when it comes to diet, and avoid following extreme diets independently, as mindful eating is essential.
- Maintaining a healthy weight is also important. Both underweight and overweight individuals may experience hormonal imbalances, which can affect fertility. Ensure you exercise regularly—walking, yoga, or light workouts can help improve blood flow and support reproductive health without placing excessive stress on the body.
- Quitting smoking, alcohol, and illicit drug use, and avoiding exposure to environmental toxins can also improve egg and sperm quality.
- Managing stress through relaxation techniques such as meditation, deep breathing, or counselling can help regulate hormones and improve overall well-being.
Consulting a doctor to identify underlying issues, such as hormonal imbalances, thyroid disorders, or conditions like PCOS or endometriosis, is essential. Following personalised treatment plans, including supplements and medications as prescribed by a doctor, can help enhance embryo quality.
© 2024 Bennett, Coleman & Company Limited

