- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
1st-Ever In-Womb Stem Cell Therapy for Spina Bifida Found Safe, Gets US FDA Backing: The Lancet
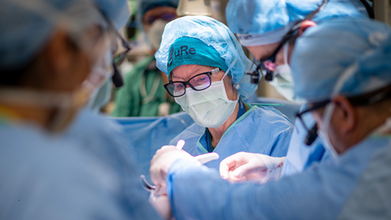
Credit: University of California-Davis Health
In a medical milestone, a team of US surgeons has deemed an in-utero surgery that adds stem cells to treat spina bifida -- a birth defect -- to be safe. This new type of fetal therapy does not just repair the defect but may also help heal and protect the baby’s developing spinal cord.
The Phase 1 clinical trial, published today in The Lancet and based on six babies, showed that adding a layer of human placenta-derived stem cells to standard fetal surgery can be done safely. The early safety results have prompted the US Food and Drug Administration (FDA), along with an independent monitoring board, to approve the next phase of the study.
Spina bifida, also known as myelomeningocele, occurs when spinal tissue fails to fuse properly during the early stages of pregnancy. The birth defect can lead to a range of lifelong cognitive, mobility, urinary, and bowel disabilities.
While surgeons have previously performed prenatal surgeries, this is the world’s first in-utero stem cell therapy for spina bifida. It is also the only clinical trial aimed at improving outcomes beyond those achieved with fetal surgery alone.
“Putting stem cells into a growing fetus was a total unknown. We are excited to report strong safety results,” said Diana Farmer, the clinical trial’s principal investigator and chair of the Department of Surgery at the University of California-Davis Health.
“It paves the way for new treatment options for children with birth defects. The future is exciting for cell and gene therapy before birth,” she added.
How The Breakthrough Fetal Surgery Was Conducted
Surgeons made a small opening in the mother’s uterus and gently positioned the fetus to expose its back and the spina bifida defect.
A small patch containing living stem cells was then placed directly over the exposed spinal cord before closing the layers of the back to allow the tissue to regenerate.
The stem cells, taken from donated placentas, are designed to protect the developing spinal cord from further damage before birth.
Treating Spina Bifida Before Birth
The findings from the first six babies in the trial, who were closely monitored from surgery through birth, revealed no safety concerns related to the stem cells.
After surgery, the babies experienced no infections or spinal fluid leaks. No abnormal tissue growth or tumors formed at the repair site.
All six surgeries were successful, and the stem cell patch was placed as planned in every case. All surgical wounds healed completely.
MRI scans also showed reversal of hindbrain herniation -- a condition commonly associated with spina bifida -- in all infants, an indicator of surgical success.
Hindbrain herniation in babies, often referred to as Arnold-Chiari II malformation, involves the lower part of the brain descending into the cervical spinal canal.
This can block the flow of cerebrospinal fluid, causing dangerous hydrocephalus (fluid buildup). None of the babies required a shunt for hydrocephalus before hospital discharge, the researchers said.
What Is Spina Bifida
Spina bifida affects about 1 in 2,500 births worldwide, with an estimated 1,500 to 2,000 babies diagnosed each year in the United States alone.
It is a common neural tube defect, with higher prevalence observed in regions with lower folic acid fortification. Open spina bifida specifically occurs in approximately 1 in every 2,875 births.
This surgical intervention aims to significantly improve motor function, and increase the likelihood of walking independently.
The first phase of the trial was funded by a $9 million state grant from the California Institute for Regenerative Medicine (CIRM).
The trial is now enrolling up to 35 patients in its Phase 1/2a study.
Children will be followed through age six to evaluate long-term safety and early signs of improved movement, as well as bladder and bowel function.
Indian Drugmakers Are Gearing Up To Launch Generic Semaglutide Injections As Weight-loss Drugs Patent Expires In March

Credits: Canva
Indian drugmaker Dr Reddy's Laboratories is now gearing up to launch its generic semglutide injection in the country in March under the brand name Obeda, reported the news wire agency Reuters. Patent protection for semglutide expires in India in March 2025. This has triggered a rush among Indian drugmakers to come up with lower-cost versions.
Semaglutide is the active ingredient in Danish drugmaker Novo Nordisk's Ozempic and Wegovy, popularly known as the weight loss drugs, but also effective for diabetes and used primarily for that.
Also Read: Scientists Develop First Antibodies To Block Epstein Barr Virus
Indian Drugmakers Rush For Generic Weight Loss Drugs
Hyderabad-based Dr Reddy's already applied for trademark with the brand name Obeda and a logo, reported Reuters, based on a government filing. In an email response to Reuters, Dr Reddy's spokesperson said, "As semaglutide is yet to be officially launched, it would not be appropriate to refer to or publish any name as the brand name at this stage."
Other companies like Sun Pharma, Zydus Lifesciences, and Nacto Pharma too are entering the rat race of launching multiple generic versions to make the treatment more affordable for patients with obesity and weight-related health risks.
Sun Pharma also announced the plans for "day-one" launches of generic prefilled pens.
Will Launching Generic Weight Loss Drugs Make It Cheaper To Buy?
Until the patent is expired, the semaglutide therapies are owned by the original company. In India, semaglutide injections like Ozempic and Wegovy are soled at a high cost that has limited accessibility to many patients.
Industry analysts, as reported by NDTV, expect that one generic semaglutide enters the market from March 21, 2026, prices could be cut roughly by 50 per cent as compared to the prices it started with. This means Wegovy which was previously sold for around Rs. 10,000 per month could fall somewhere between Rs 3,500 to Rs. 4,000 per month for starter doses.
Dr Reddy's Laboratories have positioned their generic brands competitively, and could potentially offer discounts of up to 50 to 60 per cent in early competition.
How Does Semaglutide Work?
Semaglutide works as a GLP-1 receptor agonist that mimics the GLP-1 hormone to regulate appetite and blood sugar. It slows gastric emptying and makes you feel fuller longer. It also signals the brain to reduce hunger and cravings, and triggers the pancreas to release insulin when blood sugar is high.
Read: Wegovy And Ozempic Will Cost Less In 2027, Novo Nordisk Slashes Weight Loss Drugs Prices By Half
They work by increasing insulin release in a glucose-dependent manner, decreasing the liver's production of glucagon, and slowing down the emptying of the stomach, which helps lower blood sugar levels after a meal. They also act on the brain to suppress appetite and increase feelings of fullness, leading to reduced calorie intake.
In people with type 2 diabetes, notes Harvard Health, the body's cells are resistant to the effects of insulin and body does not produce enough insulin, or both. This is when GLP-1 agonists stimulate pancreas to release insulin and suppress the release of another hormone called glucagon.
These drugs also act in the brain to reduce hunger and act on the stomach to delay emptying, so you feel full for a longer time. These effects can lead to weight loss, which can be an important part of managing diabetes.
Scientists Develop First Antibodies To Block Epstein Barr Virus
Credits: Canva
Scientists for the first time ever developed antibodies that could block Epstein Barr virus or EBV. This is a pathogen that is estimated to infect 95 per cent of the global population. The Epstein Barr virus is also linked with multiple types of cancer, neurodegenerative diseases and other chronic health conditions.
Antibodies for Epstein Barr Virus: How Does It Work?
Scientists used mice with human antibody genes. The team then developed new genetically human monoclonal antibodies that would prevent two key antigens on the surface of the Epstein Barr virus from binding to entering human immune cells.
The findings are published in Cell Reports Medicine. The study shows how the newly identified monoclonal antibodies successfully block infection in mice with human immune systems when they had EBV.
Scientists View On The Antibodies That Block Epstein Barr Virus
"Finding human antibodies that block Epstein Barr virus from infecting our immune cells has been particularly challenging because, unlike other viruses, EBV finds a way to bind to nearly every one of our B cells," explained Andrew McGuire, Ph.D., a biochemist and cellular biologist in the Vaccine and Infectious Disease Division at Fred Hutch. "We decided to use new technologies to try to fill this knowledge gap and we ended up taking a critical step toward blocking one of the world's most common viruses."
What Was the Challenge In The Creation Of Antibodies To Block Epstein Barr Virus?
The key challenge was to pursue human monoclonal antibodies that could actually halt the Epstein Barr virus infection without triggering an anti-drug response to the antibodies themselves. This is a common response among patients who are treated with antibodies raised in other animals.
The researchers targeted two antigens namely: gp350, which helps EBV bind to cell receptors. The second antigen was gp42 that allows EBV to enter and infect human antibody genes. This has led to the monoclonal antibodies to work against gp350 and eight gp42.
"Not only did we identify important antibodies against Epstein Barr virus, but we also validated an innovative a new approach for discovering protective antibodies against other pathogens," noted Crystal Chhan, a pathobiology Ph.D. student in the McGuire Lab. "As an early-career scientist, it was an exciting finding and has helped me appreciate how science often leads to unexpected discoveries."
Read: Chronic Epstein-Bar Virus: Can A Common Viral Infection Cause Fatal Brain Damage?
What Is Epstein Bar Virus (EBV)?
EBV is a highly contagious virus that can pass through bodily fluid contact. It is the cause of one of the most common infections, mononucleosis or mono. Once you get this virus, it stays in your body, inactive and in a dormant state until it becomes reactivated.
According to the Frontiers in Immunology, Chronic active Epstein-Barr virus (CAEBV) disease is a very uncommon problem where people's bodies can't fight off the EBV virus. It keeps getting worse, with a lot of the virus's DNA in their blood and the virus attacking their organs with infected blood cells.
People with this disease often have fevers, swollen glands, a big spleen, liver problems caused by EBV, or low blood counts. Over time, their body's ability to fight off infections gets weaker. If they don't get treatment, they can die from other infections, a problem where the body attacks its own blood cells, organ failure, or cancers linked to EBV.
The only treatment that has been proven to work for this disease is a stem cell transplant (a procedure to replace damaged blood cells with healthy ones). Right now, scientists are trying to figure out why this disease happens. They are looking at problems with the body's defense system (immune defects) and changes in people's genes that might be linked to the disease. A new study as also revealed that EBV may also cause us brain damage due to a disease called encephalitis.
Symptoms Of Epstein-Bar Virus
EBV infections do not cause symptoms especially for children, teens and adults are more likely to experience symptoms like fever, feeling tired or fatigued headache, sore throat, swollen lymph nodes in your neck and arm, enlarged spleen or swollen liver, body aches and skin rash. The symptoms of this usually last for two to four weeks. Things are a bit different with Chronic EBV. In rare cases of EBV, it can lead to a chronic condition called active EBV (CAEVB) some symptoms include, swollen and tender lymph nodes, fever, enlarged liver, fatigue, sore throat, headache, muscle pain joint stiffness, anemia and liver failure.
Meghalaya Health Minister Warns State Has Highest HIV-Related Deaths

Credit: Hub News
Meghalaya's Health Minister Wailadmiki Shylla has raised alarm over the rising HIV cases in the state, noting that 10,293 infected residents were receiving antiretroviral treatment.
Along with this, Shylla noted that nearly 750 people have died due to the condition in the past decade with East Khasi Hills district reporting 435 of those cases. Coming in second is West Jaintia Hills with 123 cases, East Jaintia Hills with 90 cases, Ri Bhoi with 51 cases and Eastern West Khasi Hills reporting 16.
Nine deaths in West Garo Hills, eight in West Khasi Hills, seven in South West Khasi Hills, three in South Garo Hills, two in South West Garo Hills, and one in North Garo Hills have also been recorded.
During a question hour in an assembly session on February 25, the official said: "It is very unfortunate, but Meghalaya is having the highest cases in India".
He also highlighted the confidentiality clauses in the HIV and AIDS Prevention and Control Act, 2017 as well as existing social stigma as major challenges in addressing the rampant spread of the issue. “Early detection and intervention get complicated because testing requires consent and treatment cannot be forced,” he said.
“The State government has sanctioned a ₹25-crore intervention program for the next five years to address the alarming rise in HIV/AIDS cases,” Shylla declared as well as assured that the Department has been intensifying awareness campaigns to improve testing and treatment.
The global challenge of HIV/AIDS remains one of the most pressing public health issues today. According to the latest data from UNAIDS, around 38.4 million people worldwide are living with HIV/AIDS.
As of 2024–2025, India has approximately 2.5 million to 2.56 million people living with HIV (PLHIV), marking the third-largest HIV epidemic globally, underlining the need for not only medical intervention but also comprehensive awareness, education, and social change.
What Is HIV?
HIV is the virus responsible for attacking the body’s immune system, specifically targeting CD4 cells, which are crucial for the body’s defense against infections. As HIV progresses, it destroys these cells, weakening the immune system over time. If left untreated, this continuous damage can lead to AIDS.
HIV is highly contagious and can be transmitted through the exchange of bodily fluids such as blood, semen, vaginal fluids, and breast milk. It is primarily spread through unprotected sexual contact, sharing needles, from mother to child during childbirth or breastfeeding.
Without treatment, HIV progresses through three stages:
- Acute HIV Infection: This stage occurs shortly after transmission and may include symptoms like fever, fatigue, and swollen lymph nodes.
- Chronic HIV Infection: Often asymptomatic or mildly symptomatic, the virus continues to damage the immune system but at a slower rate.
- AIDS: This is the final stage, marked by severe immune damage and the presence of infections that take advantage of the compromised immune defenses.
The disease is diagnosed through blood tests or oral swabs that detect the presence of the virus or antibodies produced by the immune system in response to the virus. Early detection of HIV is crucial, as it allows for timely intervention and treatment, which can prevent the virus from progressing to AIDS.
For HIV, the primary treatment goal is to suppress the virus to undetectable levels, thus maintaining a strong immune system and preventing further transmission of the virus. People living with HIV can often live long, healthy lives if they adhere to antiretroviral therapy (ART).
What's Happening In Mizoram?
Mizoram Health Minister Lalrinpuii has expressed serious concern about rising HIV cases, as data shows that cases in the state are 13 times higher than the national average.
Calling it a "collective disgrace", Lalrinpuii said: “About 70 per cent of HIV transmissions in Mizoram occur through sexual contact. While the national prevalence rate stands at a mere 0.2 per cent, Mizoram’s rate has climbed to 2.74 per cent. This is a matter of shame for Mizo society.”
Speaking at an event organised for International Condom Day in Aizawl on February 13, she noted that a majority of that sexual contact remains the primary route of HIV infections in the state, accounting for 70 per cent of all cases.
The minister noted that the spread is largely driven by infidelity and a lack of preventive measures, which she argued contradicted the moral and religious values of the Mizo society.
She urged the people of the state to remain faithful to their partners. “To protect the future of Mizoram, our youth must remain vigilant,” Lalrinpuii added.
© 2024 Bennett, Coleman & Company Limited

