- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Woman Left Screaming In Pain After Sex Toy 'Pulled Through Body' During MRI Scan
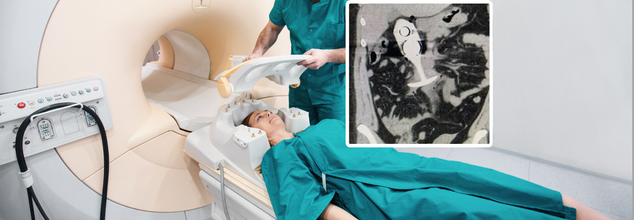
MRI scans are strong diagnostics with high-definition images of what lies inside a body. Strong magnetic fields require precaution, as brought out by an instance where a young woman suffered very serious injuries due to an oversight in a metallic core within a silicone sex toy that she happened to have before the MRI scan. This makes a stark reminder about the potentially deadly consequences of missing metal objects when such procedures are being performed. In April 2023, a 23-year-old woman went into an MRI with a silicone plug containing a metal core that was not known.
She thought that the item is made entirely out of silicone according to the advertising. However, the strong magnetic field of the MRI machine interacted with the hidden metal, dragging the object through her body and causing excruciating pain. According to reports from the U.S. Food and Drug Administration (FDA), the scene was harrowing, with the woman screaming in agony and requiring immediate hospitalization. Despite pre-scan screenings, which are routine prior to a scan, the patient did not inform the facility that the object existed because he presumed it was purely non-metallic. This caused serious injuries that led to the patient's law suit against the manufacturer for deceitful misrepresentations of material content.
MRI machines employ magnets between 0.5 to 3 Tesla (T). This is thousands of times stronger than the Earth's magnetic field. The tremendous force causes ferromagnetic materials, like iron and nickel, to be magnetized quickly and become strongly attracted toward the magnet. Objects as small as hairpins or paper clips will accelerate at 40 miles per hour inside the magnetic field.
The force can lead to catastrophic injuries in items lodged within the body, such as metallic implants or foreign objects. Metallic cores within devices, like pacemakers or intrauterine devices, must be disclosed to radiologists to prevent such complications.
How Metal Objects Interact with MRI Fields?
On these claims, Dr. Adam Taylor, a specialist in human anatomy, weighed his words in a international health website and added that the distance away and mass of this object would increase its velocity towards that of sound, "The acceleration would be phenomenal, but with a metallic core, it can't go anywhere near supersonic speeds. As for the size, the magnetic acceleration to the internal soft tissues would ensure that there could be severe intracranial trauma."
The injuries inflicted in this case likely involved damage to major blood vessels, nerves, or organs, highlighting the devastating impact of even minor oversight during an MRI scan.
This is not an isolated case. There are documented cases of metallic objects causing serious damage during MRI scans with a 65-year-old man with schizophrenia swallowed metal objects, including sockets and a hinge pin. The powerful magnetic field during an MRI scan caused the objects to rupture his stomach, resulting in serious injuries.
A toddler who ingested 11 small magnets perforated his bowel while undergoing a scan, making his case unique. In another deadly but extremely rare incident, there have been people who hide a firearm on themselves during MRI procedures. Magnetic attraction can trigger a discharge in a weapon and has led to some fatal injuries.
These cases emphasize the very strong need for adequate screening and patient education prior to an MRI.
Preventing MRI-Related Incidents
Medical professionals have been trained to avoid risks. This is by properly screening a patient for metallic objects. In general, most pre-scan protocols include:
- Patients are interrogated about implants, recent surgery or exposures at work related to metals.
- Radiologists sometimes use handheld metal detectors to search for hidden items.
- People who work with metal, like welders or machinists, will need additional testing to detect microscopic metal fragments within soft tissues or eyes.
The case emphasizes the importance of product labeling by manufacturers, especially those products that are likely to unintentionally cause harm to health. The patient's assumption that her device was 100% silicone points to a larger problem in consumer markets with misinformation.
It also reminds the patients to report any possible dangers to the medical professionals, no matter how the objects look non-metallic. In sensitive cases, patients can request private discussions with healthcare providers to ensure safety without discomfort.
In the end, it is a joint effort from manufacturers, healthcare professionals, and patients that can prevent such tragedies. Manufacturers must ensure truthful marketing, while healthcare providers should educate patients about the dangers of metal objects in MRI settings. For patients, understanding the risks and actively participating in pre-scan disclosures can be lifesaving.
This young woman's experience is a sobering example of the unforeseen dangers posed by MRI machines when precautions are overlooked. It serves as a wake-up call to address gaps in patient awareness, medical protocols, and product transparency. By learning from this incident, the medical community and the public can work together to ensure MRI scans remain a safe and effective diagnostic tool.
Ohio TikTok Star Rachel Tussey Dies After Cosmetic Surgery Complications

Credit: Gofundme.com
Rachel Tussey, a 47- year-old TikTok influencer from the US state of Ohio, has reportedly died following complications from the cosmetic “mommy makeover” surgery.
The “mommy makeover” tummy tuck procedure left her brain dead and was later pulled from life support, the New York Post reported.
Her death was confirmed by her husband, Jeremy Tussey, on March 18 through an update shared on a GoFundMe page created to support the family.
Rachel, with more than 27,000 TikTok followers, described herself as “over 40 & fabulous”. She had been documenting her story and her preparations, excitement, as well as her fear, ahead of the upcoming abdominoplasty procedure.
In her last video posted on the day of her surgery on February 25, she told her followers that she had “waited a really long time for” the procedure.
“I’m in good hands. I know God’s got my back. Let’s do this,” an enthusiastic Tussey dressed in a hospital gown said in the video.
While her surgery was successful, her husband was also able to speak with her briefly afterward. However, Jeremy informed his wife's followers that her face had gone pale, and later became unresponsive. Cincinnati.com reported.
Medical Neglect
In the GoFundMe page, Jeremy cited “medical neglect” that led to complications.
“Following the procedure, she suffered severe brain damage after extended loss of oxygen and was placed on a ventilator under sedation,” he said.
In his TikTok post, Jeremy told her followers that he believes the dose of painkillers given to his wife at the surgery center was too high.
“To me, it looks like incompetency. Somebody dropped the ball here,” the grieving husband said. “Somebody dropped the ball and killed my wife.”
Due to “very minimal brain activity”, on March 5, Jeremy took the “heartbreaking decision to remove her from life support”.
“Rachel was an amazing wife, mother, and person who touched so many lives. We will carry her memory with us always,” the page said.
She is survived by her husband and three children.
What Is Abdominoplasty?
The abdominoplasty, commonly referred to as a "tummy tuck", is a plastic surgery procedure that helps reduce excess skin and fat around the abdomen.
While it is not a weight loss solution, the procedure can help flatten the stomach and also tighten the abdominal muscles, and give an aesthetic look.
Plastic surgeons performed over 160,000 tummy tuck (abdominoplasty) procedures in the United States in 2022.
It is commonly preferred by:
- men and women desiring aesthetic improvement of the abdomen,
- women with significant skin and abdominal wall laxity following multiple pregnancies,
- bariatric patients who have excessive skin following significant weight loss.
However, patients undergoing the surgical procedure must have a good nutritional status, as well as optimal overall medical health.
Patients with a higher body mass index (BMI) and diabetes mellitus may be at significant risk post-surgery.
UK Meningitis Outbreak: Cases Rise To 20; 9-month-old Baby Battles For Life In Intensive Care

Credit: Canva
The “unprecedented” wave of meningitis outbreak in the UK's Kent, which claimed two lives, has risen to 20 cases, according to health officials.
While almost all cases have been linked to those who visited the Club Chemistry nightclub in Canterbury between March 5 and 7, a 9-month-old baby from Folkestone is reportedly battling for life in the intensive care unit.
The UK Health Security Agency (UKHSA), in a statement, noted that it is aware of a baby with confirmed Meningococcal group B infection who is not currently linked to the outbreak. The agency said it will continue to investigate the case.
The baby Nala-Rose Fletcher, from Folkestone, is currently in intensive care at Evelina London Children’s Hospital. According to doctors, she will be permanently affected by the infection, the Independent.co.uk reported.
Meanwhile, another university in the city confirmed a case of meningitis on Wednesday. The student at Canterbury Christ Church is believed to be a man who was at the nightclub and part of the 20 known cases.
“We have reached out to support the individual directly, and student wellbeing and support are reaching out and making themselves available to support fellow students more widely,” Canterbury Christ Church University said in a statement.
“We have followed UKHSA advice and informed the limited number of close contacts of the individual that they should receive precautionary antibiotics, if they have not done so already,” it added.
The Meningitis Outbreak May Have Contained
The UK health officials believe that the “unprecedented” wave of meningitis outbreak may have been “contained” as no new cluster of cases has been reported.
Health officials from the NHS, the UKHSA, and county council public health staff tackling the outbreak noted that the 20 people diagnosed with the illness have not infected anyone outside the area, the Guardian reported.
“We may have contained it. There are no cases popping up elsewhere that we know of – no cases that we know of outside the cluster – or not yet anyway,” said an official involved in the multi-agency response.
Notably, the officials have identified the outbreaks linked to a known strain of meningitis B, the report said. Six of the nine confirmed cases are group B (MenB), the agency added.
UKHSA In Prompt Action
The UKHSA has been prompt in action since the outbreak first began in Kent.
“As of 5 pm on 17 March, 9 laboratory cases are confirmed, and 11 notifications remain under investigation, bringing the total to 20. Six of the confirmed cases are confirmed to be group B meningococcal disease,” the agency said.
A 21-year-old student at the University of Kent and a teenage student at a school in the town of Faversham have died in the outbreak.
The agency has also rolled out the MenB vaccine to 5,000 students living in the University of Kent halls of residence in Canterbury.
In addition, over 2,500 doses of antibiotics -- the most effective treatment to limit the spread of invasive meningococcal disease -- has been given to students, close contacts, and others, including some of those who attended Club Chemistry between March 5 and 7.
Further, calling the illness in the Kent outbreak “severe, with rapid deterioration”, the UKHSA has issued an urgent alert to all NHS doctors in England. It advised the healthcare workers to to look for meningitis symptoms and to wear personal protective equipment before giving suspected patients antibiotics.
What is Meningococcal disease?
Caused by meningococcal bacteria, the meningococcal disease leads to inflammation of the lining of the brain also called as meningitis. The condition can also lead to sepsis or blood poisoning.
As the onset can be sudden, knowing the signs and symptoms and acting quickly is important.
Common symptoms include:
- rash
- sudden onset of high fever
- severe and worsening headache
- vomiting and diarrhoea
- joint and muscle pain
- seizures
India Played Key Role In Decline Of Child Mortality In South Asia: UN Report

Credit: UNIGME
With interventions targeted towards improving maternal and child health along with quality and accessible health infrastructure, India has played a crucial role in the decline of global child mortality, especially in South Asia, according to a UN report today.
The UN Inter-agency Group for Child Mortality Estimation (UNIGME) Report 2025 highlighted that the country's sustained efforts in the last two decades in child health have led to significant outcomes in South Asia. They include:
- a 76 percent decline in under-five deaths since 1990 and a 68 percent drop since 2000
- the under-five death rate in the region fell from 92 deaths per 1,000 live births in 2000 to nearly 32 in 2024.
"India emerges as a leading global exemplar in the UN IGME 2025 report for accelerating child mortality reduction," JP Nadda, Union Health Minister, shared in a post on X.
"India’s focussed comprehensive approach on neonatal care has paved the way for eliminating preventable child deaths and securing healthy future for our children," he added.
Also read: 4.9 Million Children Died Before Age Five Worldwide In 2024: UN Report
India's Child Health Programs
In India, the UNIGME report showed that:
- under-five mortality rate reduced to 26.6 in 2024
- infant mortality fell to 23.3 per 1000 live births
- neonatal mortality rate dropped to 17
The report lauded India’s "continuum-of-care strategy" that has integrated sustained strengthening of a vibrant health system with commensurate expansion of its health infrastructure.
It also hailed demand-driven programmatic interventions in reducing preventable maternal and newborn mortality. These include:
- Janani Shishu Suraksha Karyakram (JSSK)
- Janani Suraksha Yojana (JSY), all of which are striving towards .
- Dedicated Maternal and Child Health (MCH) wings,
- Maternity Waiting Homes,
- Special Newborn Care Units (SNCUs),
- Newborn Stabilization Units (NBSUs),
- District Early Intervention Centres (DEICs).
Further, it noted that India’s commitment to improving newborn and child survival has also been reflected in continuous quality improvement initiatives such as the recently released guidelines on Facility-Based Newborn Care (FBNC) and
digital innovations such as Tele-SNCU (HUB & SPOKE model).
These efforts are complemented by hybrid skill-based learning modules on the safe and rational use of oxygen (including CPAP) and by the empowerment of mothers and caregivers to provide nurturing care to small and sick newborns.
"India is among the first few countries to set targets and release operational guidelines on Stillbirth Surveillance and response," the report said.
The UN noted that India’s experience shows that "sustained leadership, strategic investments, and strong collaboration with committed stakeholders have enabled a robust, scalable, and effective implementation framework targeted towards the achievement of the SDGs".
© 2024 Bennett, Coleman & Company Limited

