- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Ozempic Burps Decoded: Diabetes Expert Reveals What Doctors Won’t
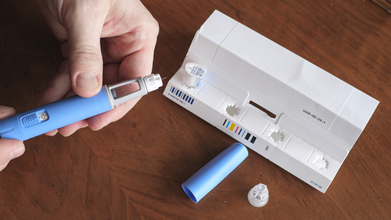
Credit: Canva
Been wondering what are Ozempic burps and how the drug works inside your body?
In a podcast episode of The Diary Of A CEO, insulin resistance expert Dr Benjamin Bikman explains how the blockbuster GLP-1 drug can alter the digestion process in your body to reduce weight.
Dr Bikman, a Professor of Cell Biology and Physiology at Brigham Young University in Utah explained: "GLP-1 is primarily a satiety hormone. It'll tell the brain that we're done eating and it will slow down the intestines significantly."
Ozempic (semaglutide) is a prescription injectable GLP-1 medication primarily approved for adults with Type 2 diabetes to manage blood sugar levels. However, the drug has gained immense popularity among those trying to lose weight as it can reduce hunger and help people feel full for longer, which forces the body to burn fat deposits to stay functional.
Also Read: UK Toddler Dies Of Rare Kawasaki Disease: What You Need To Know
In clinical trials, people with obesity using semaglutide have shown to lose an average of about 15% of their body weight over 68 weeks. Most people begin to see noticeable results within 8 to 12 weeks of taking the drug.
The official price in India for a once-weekly Ozempic injection pen ranges from approximately ₹8,800 for the 0.25 mg dose to around ₹11,175 for the 1 mg dose per month. Insurance coverage is generally inconsistent for weight loss indications.
How Does Ozempic Change Your Digestion?
According to Dr Bikman, ingested food sits in the stomach and intestines for about six hours on average for digestion. However, when the body receives GLP-1 hormones from injections, the body will considerably slow down the digestion process and food can stay in the body for about 24 hours.
"If we injected ourselves with a GLP-1 drug, which puts an artificial amount of GLP-1 in our body, boom, we shoot it in. Then it would it slows down people's intestines so much that they'll have food sitting in there for 24 hours," he said during the episode.
Experts have previously noted that slowing down the digestion process on purpose using drugs is unhealthy and risky unless done under strict medical supervision to treat a specific condition (such as chronic diarrhea or dumping syndrome as it can lead to gastroparesis.
Gastroparesis is a condition that occurs when the stomach muscles become weak and slow, failing to move food into the small intestine which can reduce nutrient absorption in the body and severe constipation. It can also form a hard mass called a bezoar, which can cause blockages and may require surgery.
What Are Ozempic Burps?
As the food continues to sit in the body, it create bubbles and gas inside the stomach which leads to intense burps also know as Ozempic burps."So, one of the things people talk about is what's called Ozempic burps where they just have this kind of belching bubbling gas because the food is sitting in the stomach for way longer than it's supposed to.
"So, no surprise the people are less interested in food. GLP-1 tells the brain they don't need to eat as much and slows down the intestines," Dr Bikman noted.
READ MORE: Wegovy 7.2 mg: Higher-Dose Weight-Loss Jab Cleared For Launch In UK
Can You Regain Your Ozempic Weight?
Yes. A new BMJ study has found that people who stop using weight-loss medications can regain weight and return their original size within two years.
Researchers have found that those who lose weight using blockbuster GLP-1 drugs such as Ozempic could regain about 0.4kg every month after quitting these treatments. In contrast, those who lost weight through exercise, diet and other factors only gained 0.1kg.
No Refrigeration Needed: New Vaccine May Expand Immunization Worldwide
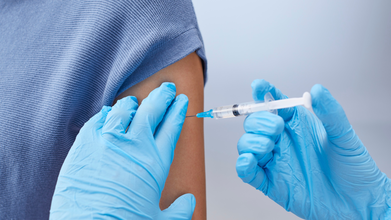
Credits: Canva
Vaccines are among the most powerful tools in modern medicine, preventing millions of deaths each year. Yet getting those vaccines safely from laboratories to people who need them is far more complicated than many realise. Most vaccines must be kept within a strict temperature range between 2°C and 8°C from the moment they are produced until they are administered.
This temperature controlled system, known as the cold chain, depends on refrigerators, insulated transport boxes and a steady supply of electricity at every step of the journey. Any disruption can damage the vaccine and make it ineffective. Now, scientists are testing a new technology that could remove this challenge altogether.
A vaccine designed to remain stable even at room temperature has shown encouraging results in an early human trial. Researchers believe this could change how vaccines are distributed, especially in regions where refrigeration is difficult to maintain.
The Challenge Of Keeping Vaccines Cold
Vaccines are sensitive biological products. Exposure to excessive heat or freezing temperatures can damage their active ingredients and reduce their ability to trigger an immune response.
To avoid this, countries rely on a carefully managed cold chain that transports vaccines from manufacturing facilities to warehouses, regional storage centers and finally to clinics. This process requires specialised equipment, trained staff and constant monitoring of temperatures.
However, maintaining this system is both expensive and complex. Equipment failures, power outages and transport delays can disrupt the cold chain at any stage. In rural or remote regions where electricity supply is unreliable, these challenges become even more serious.
Global health experts estimate that a large number of vaccines are lost every year because of temperature control failures during storage and transport. This leads to wasted doses, increased costs and gaps in vaccination coverage.
Because of these difficulties, scientists have long been searching for ways to develop vaccines that can remain effective without strict refrigeration.
A Vaccine That Can Survive At Room Temperature
One promising development is a vaccine candidate called SPVX02, which targets tetanus and diphtheria. It has been developed by the biotechnology company Stablepharma with support from the UK Health Security Agency.
What makes this vaccine different is the technology used to stabilize its active ingredients. The formulation allows the vaccine to tolerate higher temperatures without losing potency.
Early findings from a Phase I clinical trial suggest the vaccine can remain stable at around 30°C for as long as two years. The study was carried out at the Vaccine Development and Evaluation Centre in the United Kingdom and involved healthy volunteers.
Phase I trials are the earliest stage of human testing. At this stage, researchers focus mainly on safety, possible side effects and the body’s immune response.
If further trials confirm these findings, the same stabilization technology could potentially be applied to other vaccines as well.
Why This Could Matter For India
A fridge free vaccine could have major implications for countries such as India, which runs one of the largest immunization programmes in the world.
India’s Universal Immunisation Programme delivers vaccines to millions of children every year. To reach remote villages and urban settlements, the programme depends on a vast cold chain network that includes refrigerated storage facilities, specialized transport and vaccine carriers.
Maintaining this infrastructure across a country with varied climates and uneven electricity supply can be difficult. Heat exposure during transport or power failures can lead to spoilage and wastage.
A thermostable vaccine that remains effective at room temperature could simplify this process significantly. It would reduce dependence on refrigeration, lower costs and make it easier to deliver vaccines in remote or resource limited areas.
What Happens Next
Although the early results are encouraging, the vaccine still needs to go through larger clinical trials before it can be approved for widespread use.
Future studies will involve more participants and compare the new formulation with existing refrigerated vaccines to confirm its effectiveness.
If the technology proves successful, researchers believe it could be adapted for many other vaccines in the future. That possibility could reshape how immunization programmes operate worldwide and help bring life saving vaccines to communities that have long struggled to access them.
US Judge Blocks RFK Jr.’s Vaccine Schedule, Says Government Ignored Science

Credits: Wikimedia Commons
A federal judge in Massachusetts has blocked a series of vaccine policy changes introduced by U.S. Health Secretary Robert F. Kennedy Jr., dealing a significant setback to the Trump administration’s health agenda. The ruling temporarily halts new vaccine recommendations and reverses recent decisions made by the government’s vaccine advisory panel.
The decision was issued by Judge Brian Murphy of the U.S. District Court for the District of Massachusetts. It came after several medical organizations argued that the government’s actions were not based on scientific evidence and could endanger public health.
Court Says Science Was Ignored
In his ruling, Judge Murphy said vaccine policy decisions have traditionally been based on careful review of scientific data. This process is also required under federal law.
However, he wrote that the government had ignored these standards while introducing changes to vaccination guidelines. According to the court, the decisions undermined the integrity of the process that normally guides national immunization recommendations.
The ruling stops the government from implementing those changes for now. It also means the Advisory Committee on Immunization Practices, or ACIP, cannot hold its scheduled meeting this week.
Lawsuit From Medical Organizations
The case was brought by six major medical organizations, including the American Academy of Pediatrics. They claimed that the new policies changed the childhood vaccine schedule without proper scientific review.
The groups argued that the government had made “arbitrary and capricious” decisions by bypassing the usual evidence-based process. They also questioned the qualifications of several members appointed to the vaccine advisory committee.
Judge Murphy noted in his ruling that only six of the 15 committee members appeared to have meaningful experience with vaccines. The committee is responsible for recommending which vaccines Americans should receive and when.
Read: 15 States Sue Trump Administration Over Revised Vaccine Schedule
Changes to Childhood Vaccine Schedule
The lawsuit focused on a series of policy changes introduced over the past year. These included reducing the number of diseases covered under the routine childhood immunization schedule.
In January 2026, federal officials announced a new vaccine schedule that lowered the number of diseases children are routinely vaccinated against from 17 to 11.
The changes also affected recommendations for Covid vaccines. Earlier in 2025, Kennedy announced that Covid shots would no longer be recommended for healthy children or pregnant women.
Health officials supporting the changes argued that growing mistrust of vaccines had reduced vaccination rates. They believed simplifying the schedule might rebuild public confidence.
However, critics said the changes were rushed and not supported by strong scientific review.
Experts Warn About Public Health Risks
Many doctors and public health experts strongly opposed the new policies. They warned that weakening vaccine recommendations could lead to outbreaks of preventable diseases.
Medical groups say childhood vaccination programs have been one of the most successful public health efforts in modern history. Vaccines protect children from serious diseases such as measles, polio and hepatitis B.
Several organizations also filed supporting legal documents in the case, including public health experts and research groups.
Government Likely to Appeal
Officials from the Department of Health and Human Services said the government plans to challenge the ruling. A spokesperson said the administration expects the decision to be overturned.
For now, however, the court order means previous vaccine recommendations will remain in place.
Medical organizations welcomed the ruling. They said it helps restore a science-based process that has guided vaccine policy for decades and protected the health of millions of children.
Read: CDC Vaccine Schedule: Coverage Falls From 17 to 11 Diseases For Children
What Were The Changes Suggested In The Latest CDC Vaccine Schedule?
The federal health department sought to reduce the number of shots American children receive, announced that the new Centers for Disease Control and Prevention (CDC), vaccine schedule will include routine shots for 11 diseases for children. This is down from 17 diseases, which were earlier included. Jim O'Neill, who is the acting director of the CDC updated the agency's immunization schedule to reflect the changes, effective immediately.
The most controversial change is the narrowing of recommendations for several common childhood vaccines. Immunization against the following illnesses is now advised only for high-risk children or after consultation with a health care provider:
- Hepatitis A
- Hepatitis B
- Meningococcal disease
- Rotavirus
- Influenza
- Respiratory syncytial virus, or RSV
Covid-19 vaccination has also shifted to a consultation-based recommendation rather than routine use for all children.
This means shots that were once automatically given at set ages, including at birth, during infancy, and in adolescence, may now depend on individual medical discussions rather than standard guidance.
Energy Drinks Are Not A Substitute For Water In Summer, Doctors Say

Credits: Canva
Water remains the most reliable and effective way to keep the body hydrated during hot weather. However, many people have increasingly turned to energy drinks during long workdays or busy schedules, hoping to stay refreshed or energized.
Experts warn that relying on these drinks instead of water can create several health risks, particularly when temperatures are high.
Energy drinks are typically marketed as quick solutions for fatigue and low energy. They often contain high levels of caffeine, added sugars and stimulants that may temporarily increase alertness.
While this short term boost may seem appealing, experts say these drinks are not designed to support proper hydration. When consumed frequently, especially during summer, they can place extra strain on the body rather than helping it stay cool and hydrated.
Dr Arun Sachdeva, an Internal Medicine Specialist at Felix Healthcare in Bengaluru, explains that replacing water with energy drinks during hot weather can interfere with the body’s natural hydration balance.
According to him, excessive consumption of these beverages may contribute to both immediate and long term health concerns, particularly when the body is already losing fluids through sweating.
Higher Risk Of Dehydration
One of the main concerns with energy drinks is their caffeine content. Caffeine acts as a mild diuretic, which means it can increase urine production and lead to faster fluid loss from the body.During summer, when sweating already causes significant water loss, this effect may make it harder for the body to maintain proper hydration.
When energy drinks replace water intake, the risk of dehydration increases. Common symptoms of dehydration include fatigue, dizziness, headaches and dry mouth. In more severe cases, dehydration can also affect concentration, physical performance and overall wellbeing.
Excessive Stress On The Heart
Another concern is the combination of caffeine and other stimulants commonly found in energy drinks. These ingredients can raise heart rate and increase blood pressure. Regular consumption, especially in hot weather, may place additional strain on the cardiovascular system.For people who already have high blood pressure or existing heart conditions, excessive intake of energy drinks could increase the risk of heart palpitations or irregular heart rhythms. Experts therefore recommend limiting the consumption of these beverages, particularly during periods of intense heat.
High Sugar And Empty Calories
Many energy drinks available in the market contain large amounts of added sugar. Drinking them regularly instead of water can significantly increase daily calorie intake without providing meaningful nutritional value.Frequent spikes in blood sugar levels may gradually increase the risk of metabolic disorders. Over time, consistently high sugar consumption can contribute to health problems such as obesity and type 2 diabetes.
Therefore, doctors advise paying attention to sugar content in beverages, especially during hot weather when people tend to drink more fluids throughout the day.
Sleep Disruption And Energy Crashes
Although energy drinks are commonly used to combat tiredness, their high caffeine content can disrupt normal sleep cycles if consumed frequently. Poor sleep can lead to persistent fatigue, irritability and reduced concentration.Instead of providing sustained energy, regular consumption of energy drinks may lead to temporary stimulation followed by sudden drops in energy levels.
This cycle can leave individuals feeling even more tired later in the day, creating a pattern where they rely on more caffeinated drinks to stay alert.
Kidney Health And Hydration
Proper hydration plays an important role in maintaining kidney health. Water helps the kidneys filter waste products and maintain fluid balance within the body. Energy drinks do not provide the same hydration benefits when they replace water intake.When the body does not receive enough water, the kidneys may struggle to function efficiently. Over time, poor hydration can increase the risk of kidney related problems and may affect the body’s ability to regulate fluid levels effectively.
Why Water Remains The Best Choice
Doctors emphasize that water remains the safest and most effective drink for maintaining hydration during summer. It helps regulate body temperature, supports organ function and replaces fluids lost through sweating without introducing excess caffeine, sugar or stimulants.
Energy drinks may occasionally provide a quick boost of alertness, but they should not be used as a substitute for water. Maintaining regular water intake throughout the day remains one of the simplest and most effective ways to support overall health during hot weather.
© 2024 Bennett, Coleman & Company Limited

