- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Are You Taking Clonazepam? NHS Issues Urgent Safety Advice
Credits: Canva
The NHS has released updated guidance for people who are currently taking clonazepam, a commonly prescribed medicine that belongs to the benzodiazepine group. According to the health service, clonazepam is often used to control seizures or fits linked to epilepsy, ease involuntary muscle spasms, and help manage panic disorders. It is also prescribed in some cases for people with restless legs syndrome (RLS). NHS Inform notes that “around 1 in 10 people experience restless legs syndrome at some stage in their life.”
Explaining how the drug works, the NHS says it increases levels of gamma-aminobutyric acid (GABA), a chemical in the brain that has a calming effect. By boosting GABA, clonazepam can reduce anxiety, prevent seizures or fits, and relax tight or overactive muscles.
Who Can Take Clonazepam?
Clonazepam is only available on prescription and comes as tablets or a liquid. Most adults aged 18 and over can take either form. In certain cases, children as young as one month old may be prescribed clonazepam to treat epilepsy, as per NHS.
That said, there are situations where extra caution is needed. People who are due to have surgery or dental treatment, those who are pregnant, trying to conceive, or who have sleep-related conditions may be advised to stop taking the medicine. However, these are not the only groups the NHS says should be careful.
Clonazepam is not suitable for everyone. Before starting treatment, patients are advised to tell their doctor if they:
- have ever had an allergic reaction to clonazepam or any other medicine
- have myasthenia gravis, a condition that causes muscle weakness
- have sleep apnoea, which affects breathing during sleep
- have lung, liver, or kidney problems
- have spinal or cerebellar ataxia, which can cause shakiness, poor balance, and slurred speech
- have had problems with alcohol or drug use in the past
- have recently experienced bereavement, depression, or thoughts of self-harm or suicide
- have been diagnosed with a personality disorder
- are trying to get pregnant, are already pregnant, or are breastfeeding
- are due to have a general anaesthetic for an operation or dental procedure
What Are The Side Effects Of Clonazepam?
Like many medicines, clonazepam can cause side effects. Common effects, which affect more than 1 in 100 people, include disturbed sleep such as vivid dreams, feeling sleepy during the day, light-headedness, dizziness, unsteadiness, and muscle weakness.
When it comes to long-term use, the NHS warns that clonazepam can lead to withdrawal symptoms if taken for a prolonged period. Because of this risk, people who have been prescribed the drug for more than four weeks may have their dose reduced slowly when stopping treatment, rather than stopping suddenly.
The NHS also stresses that this is not a complete list of side effects. Patients are advised to read the information leaflet that comes with their medicine for full details.
Clonazepam: Serious Side Effects To Watch Out For
Although uncommon, some people may experience serious side effects while taking clonazepam. The NHS advises contacting a doctor or calling 111 immediately if you notice:
- yellowing of the whites of the eyes or skin, which may be less noticeable on darker skin tones, as this could point to liver problems
- seeing or hearing things that are not there, or believing things that are untrue
- problems with coordination or controlling movements
- swollen ankles, a fast heartbeat, coughing, and extreme tiredness, which could be signs of heart issues
- easy bruising, fatigue, nosebleeds, and breathlessness, which may indicate blood disorders
- changes in mood, such as talking more than usual, feeling unusually excited, restless, irritable, or aggressive, which are more likely in children or adults over 65
- Anyone experiencing memory problems, such as difficulty remembering things or amnesia, is advised to book an appointment with their doctor.
In rare cases, clonazepam can trigger a serious allergic reaction known as anaphylaxis.
Disclaimer: This article is for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified doctor, pharmacist, or healthcare provider before starting, stopping, or changing the dosage of any medication.
Where You Get Your Rabies Shot Matters: Doctor Explains Why Rabies Vaccines Should Not Be Given In Buttocks

Credits: Canva and screengrab from Instagram
Dr Srivanjani Santosh, Pediatrician, Social Activist and First Aid trainer, who had earlier spearheaded the ORS campaigned for eight years, urging FSSAI to ban the misuse of the term 'ORS' on non-WHO=standard sugar drinks, has once again shared an important health video on rabies vaccination. Dr Santosh shared that if any mammal, including dog, cat, horse, cow, buffalo, monkey or bat scratch or bit a person, they must be vaccinated with rabies shot.
She also pointed out something many miss: the location of administering the rabies shot. In her video she urged people to not get the shot administered in buttocks, and to only get it on their shoulders or thighs. She also claimed that many clinics and hospitals, despite knowing this fact, are administering rabies vaccination on buttocks.
Also Read: Hangover Star Ken Jeong's Wife Beats Stage 3 Breast Cancer
Why Does Location Of Administration Matter In Rabies Shot?
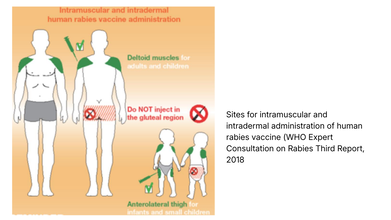
The World Health Organization (WHO) strongly recommends that rabies vaccines must be injected into the deltoid region, which is the upper arm or near the shoulder region in adults.
In small children, the WHO notes that deltoid region, as well as anterolateral area of the thigh muscle, which is also the upper thigh works.
WHO notes that like any other injections, rabies vaccine should not be given in the gluteal region, that is the buttocks, because of low absorption due to the presence of adipose or the fat tissue.
This video comes at the time when a case of a Birmingham woman losing all her limbs to dog's lick has made headlines all over the news. Health and Me also reported on the same.
Read: Woman Loses All Her Limbs After Getting Sepsis From Dog Lick
Health and Me spoke to Dr. Rakesh Pandit, Senior Consultant & HOD, Internal Medicine at Aakash Healthcare, who further explained, that as per guidelines by the WHO, the rabies vaccine should not be given in the buttocks as they have a heavy layer of fat. The body might not properly absorb the vaccine if it is injected into this fat instead of the muscle, which could result in a vaccine failure.
"A vaccine failure in case of rabies is like a death sentence because the disease is one hundred percent lethal once it shows the signs. The injection site for the vaccine depends on the patient's age; older children and adults must receive the vaccine in the upper arm or shoulder, while infants and toddlers must receive it in the thigh. The vaccine must also be administered with the right needle length to reach the required depth," he said.
Dr Pandit further elaborated, "The place of administering the vaccine (arm or thigh, subcutaneous or intramuscular) has an effect on the immune response, speed at which the vaccine is absorbed, pain and the risk of side effects." He said, "Some vaccines give best results when given in muscle for better immunity. Other vaccines may need subcutaneous administration. When given at the correct site, the vaccines ensure maximum effect, safety and reduced local reactions like swelling."
Read: 36% Of Rabies Death Comes From India: This Is What You Should Do After A Dog Bite, Explains Doctor
What Should One Keep In Mind While Getting A Rabies Shot?
Dr Mule points out that even when there are minor scratches, without bleeding, you must get a rabies shot. "Rabies can be contracted through broken skin. Such exposures still require medical evaluation and, in most cases, rabies vaccination."
What Should One Do Immediately After Being Bitten Or Scratched?
- Wash the wound immediately for at least 15 minutes with soap and running water
- Apply an antiseptic such as povidone-iodine
- Do not apply home remedies like turmeric, chili or oil
- Seek medical care promptly for rabies vaccination and possible immunoglobin
Dr Mule points out that the rabies vaccine should be started as soon as possible. "Ideally within 24 hours of a bite or scratch. However, even if there is a delay of days or weeks, vaccination should still be started immediately as rabies has a variable incubation period," he says.
The temperature of the vaccine matters. "Rabies vaccines are temperature-sensitive and must be stored between 2°C and 8°C. Exposure to heat or freezing can reduce vaccine potency. Poor cold-chain maintenance is a known reason for vaccine failure in rare cases," points out the doctor.
Dr Mule points out that the vaccine should be given intramuscularly in the deltoid or upper arms for adults, as gluteal or buttock injections could lead to inadequate absorption and reduce effectiveness.
Study Links Throat Infection To Sudden Skin Inflammation, Psoriasis
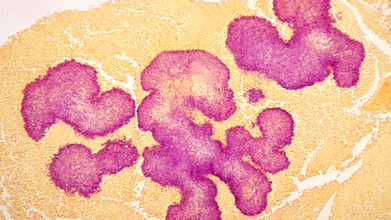
Credit: Canva
A simple strep throat infection, can trigger sudden skin inflammation, leading to psoriasis, particularly in children and young adults, according to a study.
Researchers from the Karolinska Institutet in Sweden showed that a strep throat infection caused by the Group A Streptococcus (GAS) bacterium, can trigger guttate psoriasis by altering the behavior of key immune cells. Guttate psoriasis is an often sudden-onset form of psoriasis with small, red, "drop-shaped" scaling spots on arms and legs.
While neutrophils -- the most common type of immune cell -- are the first immune cells to respond to GAS infection, the study showed that during a streptococcal infection, the immune cells behavior changes depending on their environment.
Notably, among people with guttate psoriasis, the neutrophils presented with antigens -- fragments of pathogens that signal and guide other immune cells -- get accumulated. Once accumulated, the immune cells activated the T cells, leading to inflammation, explained the researchers in the paper, published in the journal eBioMedicine.
"Doctors have long known that strep throat can precede guttate psoriasis, but the biological explanation has been unclear," said Avinash Padhi, first author of the study and Research Specialist at the Division of Dermatology and Venereology, at Karolinska.
"Our findings suggest a link between infection and skin inflammation through the accumulation of antigen-presenting neutrophils in patients' skin," Padhi added.
How Cells Shape Immune Response
The team analyzed receptor–ligand interactions -- the molecular signals cells use to coordinate immune responses to examine how neutrophils interact with other cells.Magdalini Lourda, senior author of the study and senior research specialist at the Department of Laboratory Medicine, noted that the "results challenge the traditional view of neutrophils as simple first-line defenders".
The findings show that the neutrophils play "a wider role in shaping immune responses, which may be important when designing future treatments."
How Was The Study conducted?
Using single-cell technologies, the team analyzed blood and skin samples of patients with guttate psoriasis. This enabled the researchers to examine thousands of individual immune cells in detail.To find how neutrophils work in psoriasis, the blood neutrophils from psoriasis patients were compared with those from healthy individuals. Blood neutrophils from patients with severe strep-related lung inflammation were also compared.
What Is Guttate Psoriasis?
Guttate psoriasis is a distinct form of acute-onset psoriasis. It is an inflammatory skin disease characterized by the sudden appearance of red, scaly, and smaller skin lesions widespread over the body.
The condition typically follows an infection, most commonly tonsillitis caused by Group A Streptococcus (GAS). Adolescents and young adults are the most affected. It accounts for about 2 per cent of all cases of psoriasis.
Genetics, environmental triggers, such as an upper respiratory tract infection, and the onset of an inflammatory condition in a distant organ are the major risk factors.
The condition may be diagnosed by skin biopsy, throat swab culture, and blood tests.
Hangover Star Ken Jeong's Wife Beats Stage 3 Breast Cancer

Credits: Instagram
Hangover star Ken Jeong's wife Tran Ho Jeong in 2007 discovered a hard lump in her breast while she was breastfeeding their newborn twins Alexa and Zooey. She was diagnosed with stage 3 triple negative breast cancer (TNBC) in 2008.
What Is Stage 3 Triple Negative Breast Cancer?
As per the American Cancer Society, it is an advanced aggressive, and fast-growing cancer that has spread to nearby lymph nodes or tissue, however, does not distant organs. It is characterized by the absence of estrogen, progesterone and HER2 receptors, which requires a combined approach of chemotherapy, surgery, and sometimes also radiations As per the American Cancer Society, TNBC accounts for about 10 to 15 per cent of all breast cancers.
At stage 3, TNBC has grown extensively and invaded nearby tissues and is likely to spread to lymph nodes. However, it has not metastasized to distant organs.
Also Read: Zimbabwe Among the First African Countries to Roll Out Breakthrough HIV Injections
Hangover Star Ken Jeong's Wife Cancer Journey
As doctors said, for Tran, it was a "year of hell". She underwent 16 rounds of chemotherapy when Ken was filming The Hangover. This was then followed by a mastectomy and radiation therapy.
"I am going to survive this. I am going to fight. I have to live for the girls and for Ken," she said. After two years of battle, Tran was finally declared cancer free in 2010. Ken called it "the greatest moment" of his life.
What Happens In Breast Cancer?
As per the World Health Organization (WHO), breast cancer is the most common cancer globally with around 2.3 million new cases every year. At the rate of 1 in every 8 person in both sexes and a quarter of all cancer in women with 70% mortality occurs due to constrained resources.
It is a disease where abnormal breast cells grow out of control and form tumors. If it is left unchecked, the tumors can spread throughout the body and become fatal.
It originates in the milk ducts or the milk-producing lobules of the breast. The earliest form is not life-threatening and can be detected in the early stages. Cancer cells can spread into nearby breast tissue and create tumors that cause lumps or thickening. These invasive cancers can spread to nearby lymph nodes or other organs and metastasis can be life-threatening and fatal.
Signs And Symptoms Of Breast Cancer
The common signs are:
- A breast lump or thickening, often without pain
- Change in size, shape or appearance of breasts
- Dimpling, redness, pitting or other changes in the skin
- Change in nipple appearance or the skin surrounding the nipple (areola)
- Abnormal or bloody fluid from the nipple
Treatment
The treatment depends on the stages and subtypes of the cancer. However, common treatments involve:
- Surgery to remove breast tumor
- Radiation therapy to reduce recurrence of breast cancer around the breast tissues
- Medicals to kill cancer cells and prevent spread
- Therapies like hormonal and chemotherapy or targeted biological therapy
© 2024 Bennett, Coleman & Company Limited

