- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Your Kiss Might Carry More Than Love- It Could Also Spread Anxiety, New Study Finds

Credits: Canva
Have you ever wondered if mental health could actually be contagious—just like a cold or the flu? It sounds wild, but new research suggests it might be more than just metaphorical. We’ve all heard phrases like “good vibes only” or felt someone else’s stress rub off on us, right? But what if your partner’s anxiety, depression, or even insomnia could be passed on through something as intimate as a kiss? Yep, that sweet gesture could be doing more than just bonding hearts. Intrigued? You should be—because this new finding might change how we think about emotional well-being in relationships.
A groundbreaking study out of Iran has introduced a startling new concept: that anxiety and depression may not only be shared emotionally between romantic partners—but biologically transferred through a kiss.
Yes, you read that right. Kissing your partner may not just swap affection, but millions of microbes—some of which may be quietly influencing your mental health.
This new research opens up a fascinating, and somewhat unsettling, frontier in how we understand mental wellness within intimate relationships, pointing to a biological pathway for emotional transmission through oral microbiota.
Love, Intimacy, and the Hidden Microbial Highway
It’s long been accepted that couples tend to influence each other’s behaviors—picking up habits, mimicking routines, and even adopting one another’s speech patterns. But recent scientific inquiries suggest that our bodies—and more precisely, the bacteria within them—might be syncing in much deeper ways.
A team of Iranian researchers, led by Dr. Reza Rastmanesh, followed 268 newlywed couples for six months to explore whether the oral bacteria exchanged during intimate contact—like kissing—might play a role in the development of anxiety, depression, and poor sleep.
Their conclusion? Mental health symptoms can potentially be transmitted biologically, mediated by the microorganisms that reside in our mouths.
The study, published in the journal Exploratory Research and Hypothesis in Medicine, recruited newlywed couples from two private sleep clinics in Tehran. Researchers focused specifically on couples where one spouse had been diagnosed with moderate depression, anxiety, and sleep disturbances—what the researchers referred to as the "depression-anxiety phenotype."
At the beginning of the study, the other partner was entirely healthy—no sleep complaints, no psychological distress, and no history of mental illness. Both partners provided saliva and oral swabs, which were analyzed to assess cortisol levels and map out the oral microbiota using DNA sequencing technology.
After just six months of living together, something remarkable occurred: the healthy spouses began to mirror their partners’ symptoms. Their depression and anxiety scores climbed, they reported trouble sleeping, and—most compellingly—their oral microbiomes began to resemble those of their affected partners. How could something as seemingly benign as kissing transmit psychological symptoms?
According to the study, four specific types of bacteria—Clostridia, Veillonella, Bacillus, and Lachnospiraceae—were found in higher concentrations in the saliva of affected partners. These bacteria have previously been associated with neuroinflammation and mood disorders.
When the researchers analyzed the healthy partners' microbiota after six months, they found a significant increase in these same bacteria—implying microbial transmission had occurred.
This bacterial “convergence” may play a role in disrupting the gut-brain axis, a well-documented communication system between the digestive tract’s microbiome and the central nervous system. The oral cavity is the first gateway in this axis, making these findings especially significant.
Cortisol and the Chemistry of Stress
The study didn’t stop at microbes. Researchers also tracked cortisol, a hormone released during times of stress. Healthy spouses began the study with normal cortisol levels—but after six months, levels spiked, particularly among women.
In some cases, female spouses showed nearly double the cortisol compared to their initial readings, underscoring a clear physiological stress response. This rise in cortisol mirrored the uptick in anxiety and depression symptoms, suggesting a complex chain reaction where microbial exposure leads to hormonal shifts, which in turn may affect mood.
Wy Are Women More Vulnerable?
Interestingly, gender appeared to influence susceptibility to microbial and emotional transmission. Female partners reported higher rates of mood disturbances and sleep issues than their male counterparts, despite starting the study in good mental health.
While the study does not definitively explain why women may be more affected, prior research has shown that women’s immune and hormonal systems are more sensitive to stress-related changes—potentially making them more vulnerable to shifts in microbiota and subsequent mental health symptoms.
The concept of “psychological synchrony” in relationships is not new. Previous studies have documented how couples’ heart rates, stress levels, and even reproductive hormone cycles can align over time. But this new study adds a biological layer to emotional co-regulation: one that literally lives inside our mouths.
While the idea that mental illness might be “contagious” through bacteria may sound like science fiction, it builds on a growing body of evidence linking gut and oral microbiomes to cognitive and emotional health.
“Oral microbiota transmission between individuals in close contact partially mediates symptoms of depression and anxiety,” the researchers concluded—urging the scientific community to consider bacteria as potential contributors in the mental health equation.
Of course, this study is not without its limitations. The researchers noted that they did not account for underlying health conditions, dietary habits, or genetic predispositions that may influence oral microbiota.
Still, the implications are vast. If further studies confirm these findings, oral health may become a new frontier in mental health interventions. Could probiotic therapies or personalized oral hygiene routines serve as preventive strategies for couples living with mental illness? Could clinicians someday assess microbial profiles to predict emotional risk?
Dr. Rastmanesh and his team believe this is just the beginning. They have called for more longitudinal studies to explore whether similar bacterial patterns are found in couples with longer marriages and in other mental health conditions such as bipolar disorder or post-traumatic stress.
Should You Worry About Your Next Kiss?
Not necessarily, the study doesn’t suggest we should avoid kissing or sharing close contact with loved ones. Intimacy remains a cornerstone of healthy relationships. But it does encourage us to broaden our understanding of what it means to be “in sync” with a partner—not just emotionally, but biologically.
As our knowledge of the human microbiome evolves, so too must our understanding of mental health. This study may not offer all the answers, but it raises critical questions about how deeply our relationships shape us—right down to the microscopic level.
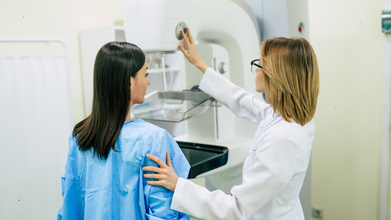
Health Tests Every Woman Should Do Once A Year
Credit: iStock
A woman’s health check-up is not about being paranoid. It's about refusing to treat your body as an afterthought.
You may not be able to control every diagnosis you ever get. But you can control how late you meet it. That's what preventive care is all about. Early detection through these screenings helps manage hormonal changes, cancer risks, and metabolic health.
From routine blood tests to specialized screenings, Dr. Supriya Bali, Director, Internal Medicine, Max Super Speciality Hospital, Saket, spoke to HealthandMe on specific tests crucial for women, right from their 20s
In Your 20s: Laying A Strong Foundation
Your 20s are all about establishing healthy habits that will carry you through life. Even if you feel great, this is a crucial time to get in the habit of seeing your doctor regularly.
Recommended screening includes:
- Blood pressure check – Every 1-2 years if normal; more often if elevated
- Pap smear – Start at age 21 (or by age 25 if you’ve never been sexually active); every three years if results are normal
- Chlamydia and gonorrhea screening – Annually for sexually active women under 25
- HPV vaccine – If not already completed by 26
- Skin check – Monitor moles and sun damage, especially if you tan easily
- Mental health screening – Don’t ignore stress, anxiety, or depression
In Your 30s: Reproductive And Preventive Health In Focus
As the body begins to undergo subtle changes in the 30s, regular screenings, hormonal health checks, and lifestyle adjustments are increasingly important.
Recommended screenings in 30s include:
- Pap + HPV co-test – Every 5 years starting at 30 (or Pap every 3 years)
- STI screening – Based on risk factors and symptoms
- Blood pressure and cholesterol check – Especially if you have a family history
- Blood sugar test – Especially if you’re planning a pregnancy or have had gestational diabetes
- Breast exam – Regular self-monitoring and breast ultrasound if you suspect a lump.
- Mental health and sleep – Ongoing check-ins with your doctor
- Fertility discussions – If you're planning or delaying pregnancy
Also read: 'Husband Stitch': A Medical Necessity Or Just A Tool To Objectify Women's Bodies?
In Your 40s: Monitoring Long-Term Risk Factors
This is a time when early signs of chronic conditions may start to show up, especially if there’s a family history of heart disease, diabetes, or cancer.
You should get these screenings at certain times:
- Mammography screening: Begin at 40 years of age (earlier if you have a family history of breast cancer).
- Pap smear & HPV test: Pap and HPV every 5 years or Pap alone every 3 years.
- Cholesterol & Blood Pressure Testing: Every 1-2 years.
- Blood glucose test (diabetes screening): especially if you're overweight or at risk for diabetes.
- Thyroid function testing is optional—especially if you feel tired, cold, or have been losing weight or have changes in your bowel habits.
- Weight discussions regarding healthy nutrition and active lifestyle—assist with maintaining a healthy weight.
- Perimenopause begins in your 40's; if you experience mood swings or changes in sleep, hot flashes, or irregular cycles, please speak with your doctor.
Also read: What Your Mammogram Says About Your Heart?
In Your 50’s: Maintain Strength, Stay Ahead of Aging
Maintaining your strength, the ability to prevent illness/disease from affecting you, and remaining proactive against the challenges that arise due to aging will be your focus at this stage.
Every individual will have their own unique series of recommended screenings; however, everyone will benefit from some type of recommended screening.
Some commonly recommended screenings include:
- Mammogram screening program; every 1-2 years.
- Colorectal cancer screening, beginning at age 45 through age 75.
- Bone density scan-if at high risk.
- Hearing/Vision checks annually or as required (on an as-needed basis).
- Blood pressure, cholesterol, and diabetes screening every year.
- Lung cancer screening among those with a history of smoking.
- Vaccines--including shingles, pneumonia, flu, and COVID-19 booster.
- Cognitive screening - to discover memory concerns, changes in mental sharpness, or cognitive function.
Silent Deficiency, Rising Risk: Why Protein May Be The Missing Link In Diabetes Care

Credit: Canva
On most clinic days, I meet patients who are doing what they believe is “everything right” for their diabetes—avoiding sweets, switching to brown rice, walking regularly. Yet their blood sugar remains stubbornly high, and complications quietly advance. When we look closer, the problem is often not just what they are cutting out, but what they are missing.
This is where the story changes. In the larger conversation on diabetes, protein rarely takes center stage. But it should.
India’s Diabetes Burden: Looking Beyond Sugar
India continues to carry one of the world’s largest burdens of Type 2 diabetes. Urban lifestyles, reduced physical activity, and easy access to refined carbohydrates have all played their role. Public messaging has, understandably, focused on reducing sugar intake.
But diets are not built on sugar alone. In countless Indian homes, especially those of vegetarians and people with limited means, the bulk of the diet revolves around cereals. Rice, wheat, or millets dominate the plate.
Protein, on the other hand, tends to be an afterthought. This creates a subtle but important imbalance: a high intake of carbohydrates coupled with insufficient protein. It's a problem that seldom gets much attention, yet it has a profound impact on metabolic health.
Understanding the Real Culprit: Insulin Spikes
To grasp the significance, let's break down the post-meal process. Eating foods high in carbohydrates, particularly those that are refined, causes a swift influx of glucose into the bloodstream. The body's response is to release insulin, a hormone that facilitates the transport of glucose into cells. While occasional spikes are perfectly normal, frequent and repeated ones put a strain on the system.
As the years pass, our cells start to ignore insulin's signals. This phenomenon, insulin resistance, is the primary problem in Type 2 diabetes. In response, the pancreas kicks into overdrive, cranking out extra insulin to try to keep up. However, this increased demand takes its toll. This slow decline in pancreatic function is what fuels the disease's advancement and opens the door to further health issues.
Also read: Diabetes Diet Plan: South Indian Breads That Are Better Than Roti
Protein: The Quiet Regulator
Now, where does protein fit into this? Protein does not cause sharp rises in blood sugar. In fact, when included in meals, it acts as a natural regulator. It slows down how quickly the stomach empties, meaning glucose enters the bloodstream more gradually. It also promotes a sense of fullness, reducing the tendency to overeat.
More importantly, protein helps maintain muscle mass—and muscle is one of the body’s largest sites for glucose utilization. Simply put, healthier muscles mean better sugar control.
A meal that includes adequate protein alongside carbohydrates behaves very differently from one that is carb-heavy and protein-poor.
The Invisible Problem: Hidden Protein Deficiency
Protein deficiency is not always obvious. Many individuals appear well-fed, even overweight, yet lack adequate protein at a cellular level. This is often referred to as “hidden malnutrition.”
In people living with diabetes, this becomes particularly concerning.
Low protein intake contributes to gradual muscle loss, especially with ageing. This loss—known as sarcopenia—reduces metabolic efficiency and worsens insulin resistance. Recovery from illness slows down. Wound healing becomes less effective. The body, in a sense, loses its resilience.
Also read: Shift to Plant-Based Proteins, Low-Fat Dairy To Boost Heart Health: American Heart Association
When Deficiency Meets Disease: A Compounding Risk
Diabetes is not just about blood sugar numbers; it is about long-term impact.
When protein intake is inadequate, the risks multiply. Nerve damage becomes more likely. Kidney health may deteriorate faster. Physical strength declines, increasing frailty and reducing quality of life.
There is also a vicious cycle at play. Reduced muscle mass leads to poorer glucose control, which in turn accelerates further muscle breakdown. Breaking this cycle requires more than medication—it requires nutritional correction.
Also read: 1 In 4 Diabetic Patients in India Suffer from Liver Fibrosis, Finds Lancet Study
How Much Protein Do We Really Need?
For most healthy adults, daily protein needs are modest but essential—roughly 0.8 grams per kilogram of body weight.
In individuals with diabetes, requirements are often slightly higher, around 1.0 to 1.2 grams per kilogram per day. However, this must always be individualized, especially in those with kidney disease or other medical conditions.
The key message is not excess, but adequacy—and consistency.
Making It Practical: The Indian Plate Reimagined
The good news is that improving protein intake does not require expensive supplements or drastic dietary changes.
For vegetarians, traditional foods offer excellent options: dals, chickpeas, kidney beans, paneer, curd, soy products, nuts, and seeds. For those who consume non-vegetarian foods, eggs, fish, and lean meats provide high-quality protein.
The simplest strategy is also the most effective: ensure that every meal contains a meaningful source of protein.
A bowl of dal with lunch, a serving of curd with dinner, or an egg at breakfast—these small additions can create a measurable difference over time.
Also read: What Is The Viral ‘Boy Kibble’ Trend?
Beyond Diet: Completing the Picture
Nutrition does not work in isolation. Regular physical activity—particularly resistance exercises—helps preserve and build muscle mass, enhancing insulin sensitivity. Adequate sleep supports hormonal balance. Stress management prevents metabolic disruptions that worsen glycemic control.
Diabetes care is not a single intervention; it is a continuum of daily choices.
Conclusion: Rethinking What We Prioritize
For too long, diabetes management has been framed as a battle against sugar alone. While reducing excess carbohydrates remains important, it is only half the story.
The other half lies in restoring balance. Addressing the protein gap offers a simple, accessible, and powerful tool to stabilize blood sugar, protect muscle health, and reduce long-term complications.
Protein is not just another nutrient on the plate. In the context of diabetes, it is part of the treatment itself.
Can Screens Rewire Your Toddler's Brain? Virtual Autism Explained

Virtual autism must not be confused with autism spectrum disorder (ASD). (Photo credit: iStock)
In today’s digital age, screens have become almost inseparable from daily life—even for very young children. While technology offers convenience and learning opportunities, increasing clinical observations have raised concerns about a phenomenon often referred to as “virtual autism." In an interview with Health and Me, Dr Aarti Javeri Manek, Paediatric Neurologist at Sir HN Reliance Foundation Hospital, explained what virtual autism is and the impact of screen time on children's brain health.
What is “virtual autism”?
Virtual autism is not a formally recognised medical diagnosis but rather a descriptive term used for children—typically toddlers—who exhibit autism-like features in the context of excessive screen exposure, particularly during critical periods of brain development. These children may show reduced eye contact, delayed speech, poor social interaction, and limited responsiveness to their environment.
Also Read: Cancer Is The 10th Leading Cause Of Death In Indian Children: Study
However, it is crucial to distinguish this entity from clinical Autism Spectrum Disorder (ASD). ASD is a neurodevelopmental condition, often with a strong underlying genetic and biological basis, present in addition to exogenous influences. External stimulus exposure may not even be apparent. In contrast, children with virtual autism often demonstrate significant improvement when screen time is reduced and replaced with real-world, interactive experiences. This reversibility is a key differentiating factor.
Read more: Is My Child Shy Or Autistic? Psychiatrist Shares Tips To Help Parents Spot Early Signs
What early signs should parents watch for?
From a neurological perspective, early childhood is a period of rapid synaptic growth, heavily influenced by sensory and social input. When screens replace human interaction, this can impact language acquisition, attention, and social interaction.
Some red flags that may suggest screen-related developmental delays include:
- Limited or absent eye contact
- Reduced response to name
- Delayed speech or loss of previously acquired words
- Preference for screens over people
- Decreased or limited gestures (not pointing, showing, or sharing interest)
- Repetitive behaviours such as watching the same videos excessively or viewing the same rhyme persistently
- Irritability or meltdowns when screens are removed
While these signs overlap with autism, the context is important. A history of prolonged, unsupervised screen exposure, often exceeding 3–4 hours per day in toddlers, should prompt consideration of environmental impact.
Read more: Can Cell Therapy Be The Future Of Autism Treatment?
Are toddlers at greater risk compared to older children?
Yes, significantly so. The first three years of life are critical for brain development, particularly for language, social bonding, and emotional regulation. During this period, the brain relies heavily on serve-and-return interactions—a child babbles, a caregiver responds; a child points, and a parent names the object. These exchanges build neural circuits essential for communication and cognition.
Screens, even educational ones, are inherently passive. They do not adapt in real time to a child’s cues in the same way a human does. Excessive exposure during this sensitive window can therefore displace meaningful interactions, leading to significant developmental delays.
Older children, while not immune, are generally more resilient, as they have already established foundational social and language skills. However, excessive screen time in this group may still contribute to attention difficulties, behavioural issues, and reduced social engagement.
What can parents do?
The encouraging aspect of virtual autism is its potential reversibility if it is identified early. Reducing screen exposure, especially in children under 2 years, and reintroducing interactive play, storytelling, and face-to-face communication may lead to noticeable improvements. Ultimately, screens are tools and not substitutes for relationships. In early childhood, it is these relationships that shape the developing brain most profoundly.
© 2024 Bennett, Coleman & Company Limited

